Research Findings
#24: Utilization and Expenditures for Children with Special Health Care Needs
Frances M. Chevarley, PhD, Agency for Healthcare Research and Quality
This report provides estimates of medical care utilization and expenditures for children with special health care needs. Presented data are from the 2000 Medical Expenditure Panel Survey (MEPS), which collects nationally representative data on health care use, expenditures, source of payment, insurance coverage, and the quality of care for the U.S. civilian noninstitutionalized (community) population and which is sponsored by the Agency for Healthcare Research and Quality and the National Center for Health Statistics (NCHS). Studying health care needs, access, utilization and expenditures for children with chronic conditions has always been difficult due to the low prevalence of most health conditions for children (Perrin, 2002; Bethel, Read, Stein, et al., 2002; Mangione-Smith, McGlynn, 1998). To address this problem, a standard definition of children with special health care needs (CSHCN) was developed (Bethel, Read, Stein, et al., 2002; McPherson, Arango, Fox, 1998) and a CSHCN screener questionnaire (Bethel, Read, Stein, et al., 2002) was created to identify these children in surveys. Because AHRQ was mandated to measure health care quality for a national quality report starting in 2003, a number of enhancements to measure health care quality were added to MEPS, including a parent-administered questionnaire (PAQ), which was added to the 2000 MEPS. The CSHCN screener questionnaire was included in the 2000 MEPS PAQ and is used to identify CSHCN for this report. It uses the Maternal and Child Health Bureau’s broad definition (McPherson, Arango, Fox, et al., 1998): “Children with special health care needs are those who have or are at increased risk for a chronic physical, developmental, behavioral, or emotional condition and who also require health and related services of a type or amount beyond that required by children generally.”
This report provides estimates according to special health care need (SHCN) status. These estimates include demographic and other personal or family characteristics of the child, health care utilization and expenditures, and burden of child’s health care costs upon the family (out-of-pocket medical expenditures for the child as a percentage of family income). Health care utilization estimates include percentage of children with ambulatory visits (office-based medical provider services plus hospital outpatient services), emergency department visits, hospital inpatient discharges, and prescription medicines. Expenditure estimates include percentage of children with total and with out-of-pocket expenditures along with average and median total and out-of-pocket expenditures according to selected characteristics of the child. In addition, the percentage distribution of out-of-pocket expenses for child’s health services as a percentage of family income is presented according to the characteristics of the child.
All differences discussed in the text are significant at the 0.05 level or better. No adjustments were made to compensate for the number of comparisons provided in this report. The technical appendix defines children with special health care needs in more detail and provides detailed information about the estimates and methods used in the report.
^top
Demographic and other characteristics of children according to SHCN status
Demographic and other characteristics of children with special health care needs (SHCN) are presented in tables 1 and 2. Overall, 16.2 percent of all children under age 18 (11.7 million children in the U.S. civilian noninstitutionalized population) were reported by their parents to have special health care needs (table 1). The prevalence of having SHCN is greater for older children than for younger children. An estimated 20.1 percent of children ages 12–17 were reported by their parents to have special health care needs compared to 10.4 percent of children less than 6 years of age. According to MEPS data, Hispanic children were less likely than both non-Hispanic black and non-Hispanic white children to have their parents report SHCN, and non-Hispanic white children were most likely to have their parents report SHCN. The prevalence of SHCN was greater for boys than for girls. An estimated 19.1 percent of boys were reported by their parents to have SHCN compared to 13.2 percent of girls. No statistically significant associations were found of SHCN status by region, metropolitan statistical area (MSA) status, or by income. There were, however, associations of SHCN status by insurance and by health status. Children reported as being without SHCN were twice as likely to be uninsured as children with SHCN. An estimated 9.3 percent of children without SHCN were uninsured compared to an estimated 4.7 percent of children with SHCN (table 2). As expected, poorer health status was associated with SHCN status. Children with SHCN were less likely than children without SHCN to be reported in excellent health (31.2 percent versus 54.3 percent), and were more likely to be reported in good (27.3 percent versus 13.9 percent) or in fair/poor health (8.1 percent versus 0.9 percent).
Health care use by SHCN status
By definition, children with SHCN are those children that “. . . require health and related services of a type or amount beyond that required by children generally” (McPherson, Arango, Fox, et al., 1998); it is not surprising, then, that children with SHCN were more likely than children without SHCN to have ambulatory visits (83.3 percent versus 67.4 percent), emergency department visits (16.3 percent versus 11.1 percent), inpatient hospital stays (6.0 percent versus 2.4 percent), dental visits (50.3 percent versus 44.2 percent), and prescription medicines (78.7 percent versus 45.8 percent) (table 3). Of children with ambulatory visits, children with SHCN have more than twice as many visits on average as children without SHCN (average of 8.2 visits per child with SHCN with visits versus an average of 3.2 visits per child without SHCN with visits). There was no statistically significant difference between children with and without SHCN status in average number of visits for children with visits for emergency department visits (1.3 average number of visits for both children with and without SHCN with visits) and for dental visits (2.6 average number of visits for children with SHCN, 2.8 average number of visits for children without SHCN). Regarding prescription medications, children with SHCN with prescriptions had three times the number of prescriptions on average as children without SHCN with prescriptions (8.7 versus 2.7).
Expenditures by SHCN status
In 2000, approximately 60.2 million children in the U.S. community population had health care expenditures of about $67 billion. Although children with SHCN make up only 16.2 percent of the population, these children accounted for 41 percent of total expenditures. Table 4 shows the percentage of children with expenses along with average and median expenditures for those with expenses according to SHCN status and according to selected characteristics. Young children (ages 0–5) were more likely to have medical expenses (87.5 percent) than children ages 6–11 (81.0 percent) or children ages 12–17 (80.9 percent). By race/ethnicity, white non-Hispanic children (88.1 percent) were more likely to incur medical expenses than both Hispanic children (74.1 percent) and black non-Hispanic children (71.9 percent). Those children living in the Northeast and Midwest were more likely than children living in the South and West to have medical expenses (89.3 percent and 87.1 percent versus 79.7 percent and 79.5 percent, respectively). Having medical expenses was positively associated with income category —the higher the family income category, the more likely the child was to have medical expenses. Health insurance also played a role in having medical expenses. Children with private insurance were the most likely to have medical expenses (87.3 percent) followed by children with public only insurance (80.0 percent); uninsured children were the least likely to have medical expenses (57.3 percent). As would be expected, children with reported fair/poor health were more likely to have medical expenses (94.7 percent) than children with reported good health (81.7 percent), very good health (84.2 percent), and excellent health (82.4 percent).
Again, due to the definition of children with special health care needs, children with SHCN were more likely than children without SHCN to have medical expenses (93.5 percent versus 81.2 percent). For each of the subpopulations in table 4 (except children under 6 years of age where the difference was not significant), children with SHCN were more likely than children without SHCN to have health care expenses.
For children with expenses, the average medical expense per child in 2000 was $1,114.62. The average medical expense for children with SHCN with expense was $2,497.84, more than three times the average medical expense of $803.12 for children without SHCN with expense. For each of the subpopulations with medical expenditures in table 4, children with SHCN had higher average medical expenses than children without SHCN. In 2000, the average medical expense for children less than 6 years with SHCN and with expense was $4,306.16, 6.5 times the estimated average expense of $663.87 for similarly aged children without SHCN and with expense.
Among those with medical expenses, average medical expenses are generally much higher than median medical expenses due to a very small group of the population having a disproportionate share of overall health care costs (Ezzati-Rice, Kashihara, Machlin, 2004). The average medical expense in 2000 for all children with expense of $1,114.62 was 3.5 times the median medical expense of $316.29 for children with expense. This large difference between average and median medical expense among those with expense is seen for both children with SHCN and children without SHCN ($2,497.84 and $695.05 for children with SHCN, $803.12 and $270.85 for children without SHCN). Similar to the pattern of average medical expenses for children with and without SHCN, the median medical expense of $695.05 for children with SHCN and expense was 2.6 times the median medical expense of $270.85 for children without SHCN and expense. For each of the subpopulations with expense in table 4, children with SHCN had median medical expenses that were two to three times the median expenses of children without SHCN.
Out-of-pocket expenditures by SHCN status
Out-of-pocket expenses are a better indicator than total medical expenditures of individual and family financial burden resulting from medical care. The percentage of children with out-of-pocket expenses is less than the percentage with total medical expenses due to health care coverage and other programs. In 2000, an estimated 70.5 percent of children had some out-of-pocket expenses for personal health services in 2000 (table 5), less than the 83.1 percent of children with medical expense (table 4). Having out-of-pocket expenses varies by demographic and other characteristics of children. Children ages 6–11 were less likely than younger and older children to have some out-of-pocket expenses (66.9 percent for ages 6–11, compared with 73.1 percent for ages 0–5, and 71.4 percent for ages 12–17). White non-Hispanic children (79.2 percent) were more likely than both black non-Hispanic children (50.8 percent) and Hispanic children (57.1 percent) to have out-of-pocket expenses. Having out-of-pocket expenses increased with family income from 46.1 percent of all children in poor/near poor families, to 63.0 percent of children in low income families, to 76.2 percent of children in middle income families, to 86.1 percent for children in high income families. Children living in the Northeast were more likely to have out-of-pocket expenses then children living in the South and West (77.6 percent versus 67.8 percent and 65.4 percent respectively). Health insurance also plays a role in whether or not children have out-of-pocket expenses. Children with public only insurance were least likely to have out-of-pocket expenses (42.2 percent), followed by uninsured children (54.7 percent)(who were less likely to use services and have any expense); children with private insurance were the most likely to have out-of-pocket expenses (81.3 percent). As might be anticipated, children with fair or poor health were more likely than other children to have out-of-pocket expenses (79.9 percent of children with fair/poor health, compared with 66.9 percent of children with good health, 71.6 percent of children with very good health, and 70.5 percent of children with excellent health).
When comparing out-of-pocket expenses for children with and without SHCN, children with SHCN were more likely than children without SHCN to have out-of-pocket expenses; 83.8 percent of all children with SHCN had out-of-pocket expenses compared with only 68.0 percent of children without SHCN. For each of the subpopulations in table 5, the percentage with out-of-pocket expenses was greater for children with SHCN than for children without SHCN.
For children with out-of-pocket medical expenses, the average out-of-pocket expense per child in 2000 was $285.60. Average out-of-pocket medical expenses increased with age from $134.91 for children ages 0–5 years, to $277.65 for children ages 6–11 years, to $450.87 for children ages 12–17 years. Average out-of-pocket expenses were higher for white non-Hispanic children ($328.12) than for Hispanic children ($194.87) and black non-Hispanic children ($154.68). Children from poor/near poor families had lower average out-of-pocket medical expenses ($163.80) than children from low, middle, and high income families ($264.95, $296.22, and $331.44, respectively). By insurance status, children with public only insurance had lower average out-of-pocket medical expenses ($160.52) than children with private insurance ($300.13) and uninsured children ($355.14). For children with out-of-pocket medical expenses, children with SHCN had higher average out-of-pocket expense than children without SHCN for each of the subpopulations in table 5, except for black non-Hispanic children, children living in the Northeast, children living in poor families, children with public only insurance, and children reported to be in excellent health, where the differences were not statistically significant.
The average out-of-pocket expense for all children with out-of-pocket expense was 3.5 times the median out-of-pocket expenses for children with out-of-pocket expense (average out-of-pocket expense of $285.6, median out-of-pocket expense of $82.75). In 2000, the median out-of-pocket expense for SHCN children with out-of-pocket expense was 2.2 times that for children without SHCN and expense ($162.05 versus $72.26). For each of the subpopulations in table 5 with out-of-pocket medical expense, median out-of-pocket medical expenses were higher for children with SHCN than for children without SHCN except for children living in the West and children in poor families, where the differences were not statistically significant.
Out-of-pocket expenditures as a percentage of family income by SHCN status
Child’s out-of-pocket expenditures as a percentage of family income is often used as a measure of burden that child’s medical expenses places on families’ income (Taylor, Banthin, 1994). The distribution of the child’s out-of-pocket medical expenses as a fraction of family income according to the child’s characteristics is analyzed in table 6. Because there are so few children with burden above 5 percent of family income, that is the top category in our tables. It should be noted that out-of-pocket expenses do not include premiums for health insurance coverage. Of the 72.4 million children in 2000, 17.6 percent of their families either had no income or no medical expense. The vast majority of children were from families with income and had out-of-pocket expense less than 1 percent of their family income (72.8 percent of all children). An estimated 4.6 percent of children had out-of-pocket expenses greater than or equal to 1 and less than 2 percent of family income, 3.2 percent of children had burden greater than or equal to 2 percent and less than 5 percent, and 1.7 percent had burden greater than 5 percent of family income. By age, older children (ages 12–17) had higher out-of-pocket expenses as a percent of family income than younger children (ages 0–5 and 6–11). An estimated 8.5 percent of older children (aged 12 years or more) had their families spend at least 2 percent of their family income on their health care compared with 2.8 percent of children ages 0–5 and 3.7 percent of children ages 6–11. Children not living in MSAs were more likely than children living in MSAs to have their families spend 2 percent or more of their family income on the child’s medical expenses. In 2000, 7.2 percent of children not living in MSAs had their families spend 2 percent or more of their family income for the child’s health care compared with 4.5 percent of children living in MSAs. Children in families with high income were less likely than other children to have their families spend 2 percent or more of their family income on the child’s medical care (2.4 percent of children in high income families versus 7 percent of children in poor/near poor and low income families and 4.7 percent of children in middle income families). Children with public only insurance were less likely to have their families spend 2 percent or more of their income on their child’s medical care (3.3 percent) than uninsured children ( 8.1 percent) and children with private insurance (5.1 percent). By SHCN status, children with SHCN were almost three times more likely than children without SHCN to have their parents spend 2 percent or more of their family income on their health care. In 2000, 10.4 percent of children with SHCN had their parents spend 2 percent or more of family income on their child’s medical care compared with only 3.7 percent of children without SHCN. Children with SHCN were more likely to have their families spend at least 2 percent of the family income on their child’s health care than children without SHCN for all of the subpopulations in table 6 (except for black non-Hispanic children, children living in the Northeast, children with public only insurance and children reported to be of excellent health, where the differences were not statistically significant).
Among children with SHCN, children not living in MSAs were more likely than children living in MSAs to have their families spend 2 percent or more of their income on their child’s health care (14.4 percent versus 9.5 percent). Also among children with SHCN, children living in poor families and those living in low income families were more likely to spend at least 2 percent of their family income on their child’s health care (15.2 percent and 13.8 percent, respectively) than children living in high income families (6.3 percent).
^top
According to the CSHCN screener instrument in MEPS, an estimated 16.2 percent of all children under age 18 (11.7 million children in the U.S. civilian noninstitutionalized population) were reported by their parents to have SHCN in 2000. Findings show that older children (ages 611 and 1217) were more likely to have SHCN reported than young children (ages 06)18.1 percent and 20.1 percent, respectively, for ages 611 and 1217 compared with 10.4 percent for ages 06. Hispanic children (10.3 percent) were less likely than black non-Hispanic children (14.8 percent) who in turn were less likely than white non-Hispanic children (18.7 percent) to have SHCN reported. Not surprisingly, among children with respective visits and use, those with SHCN had on average more ambulatory visits and more prescriptions than children without SHCN. The average medical expense for children with SHCN with expense was $2,497.84, more than three times the average medical expense of $803.12 for children without SHCN with expense. The median medical expense of $695.05 for children with SHCN and expense was 2.6 times the median medical expense of $270.85 for children without SHCN and expense. Children with SHCN were also more likely than other children to have out-of-pocket expenses; 83.8 percent of children with SHCN had out-of-pocket expenses compared with only 68.0 percent of children without SHCN. For children with out-of-pocket expenses, the median out-of-pocket expense for children with SHCN was more than twice that for children without SHCN ($162.05 versus $72.26). When analyzing the distribution of childs out-of-pocket medical expenses as a fraction of family income, children with SHCN were more likely to have their parents spend more of their family income on their childs health care than children without SHCN. An estimated 10.4 percent of children with SHCN had their families spend at least 2 percent of their family income on the childs medical care compared with only 3.7 percent of children without SHCN. Among children with SHCN, those not living in MSAs were more likely than children living in MSAs to have their families spend 2 percent or more of their income on their childs health care (14.4 percent versus 9.5 percent). Also among children with SHCN, children living in poor/near poor families and those living in low income families were more likely to have their families spend at least 2 percent of their family income on their childs health care than children living in high income families (15.2 percent of poor/near poor children and 13.8 percent of low income children versus 6.3 percent of high income children).
^top
Bethel CD, Read D, Stein REK, Blumberg SJ, Wells N, Newacheck PW. Identifying Children with Special Health Care Needs: Development and Evaluation of a Short Screening Instrument. Ambulatory Pediatrics, Vol. 2, No. 1, JanuaryFebruary 2002.
Cohen J. Design and methods of the Medical Expenditure Panel Survey Household Component. Rockville (MD): Agency for Health Care Policy and Research, 1997. MEPS Methodology Report No. 1, AHCPR Pub. No. 97-0026.
Cohen SB. Sample design of the 1997 Medical Expenditure Panel Survey Household Component. Rockville (MD): Agency for Healthcare Research and Quality, 2000. MEPS Methodology Report No. 11, AHRQ Pub. No. 01-0001.
Cohen SB. Design strategies and innovations in the Medical Expenditure Panel Survey. Medical Care, 2003, 41(7):512.
Ezzati-Rice TM, Kashihara D, Machlin SR. Health care expenses in the United States, 2000. Rockville (MD): Agency for Healthcare Research and Quality, 2004. MEPS Research Findings No. 21, AHRQ Pub. No. 04-0022.
Machlin SR, Taylor AK. Design, methods, and field results of the 1996 Medical Expenditure Panel Survey Medical Provider Component. Rockville (MD): Agency for Healthcare Research and Quality, 2000. MEPS Methodology Report No. 9, AHRQ Pub. No. 00-0028.
Mangione-Smith R, McGlynn EA. Assessing the quality of health care provided to children. Health Services Research, 1998 October, 33(4 Pt 2):105990.
McPherson M, Arango P, Fox H, Lauver C, McManus M, Newacheck PW, Perrin JM, Shonkoff JP, Strickland B. A new definition of children with special health care needs. Pediatrics, 1998 July, 102(1 Pt 1):13740.
Perrin JM. Health Services Research for Children with Disabilities. Milbank Quarterly, Vol. 80, No. 2, 2002.
Taylor A, Banthin J. Changes in out-of-pocket expenditures for personal health services: 1977 and 1987 (AHCPR Pub. No. 940065). National Medical Expenditure Survey Research Findings 21, Agency for Health Care Policy and Research. Rockville, MD: Public Health Service, July 1994.
Zuvekas SH, Cohen JW. A guide to comparing health care expenditures in the 1996 MEPS to the 1987 NMES. Inquiry, 2002 Spring, 39(1):7686.
^top
The data for this report were obtained from the 2000 Medical Expenditure Panel Survey (MEPS), an ongoing annual survey of the civilian noninstitutionalized population of the United States that collects detailed information on health status, health care use and expenditures, health insurance, access, quality, and general demographic and economic information. Expenditure data in MEPS are obtained from both the household interview and the Medical Provider Component. The Medical Provider Component collects expenditure data from a sample of respondents hospitals, physicians, home health care providers, and pharmacies. More information about MEPS can be found at http://www.meps.ahrq.gov. Detailed descriptions of the survey and its methodology have been previously published (Cohen JW, 1997; Cohen SB, 2000; Cohen SB, 2003). For additional information about MEPS expenditure data, see Ezzati-Rice, Kashahara, and Machlin (2004).
More specifically, childrens special health care needs status data are based on information collected in the 2000 parent administered questionnaire (PAQ), a paper-and-pencil parent-administered questionnaire that was distributed in late 2000 to parents of children in MEPS less than 18 years of age as of July 1, 2000. Data for this report are from the 2000 Full Year Consolidated File (HC-050) to which was added a family income variable. A special age variable (AGEJUL01) on this file indicates age as of July 1, 2000. A special weight variable (SQPQW00F) has been designed to be used with data from the PAQ for children whose July 1, 2000 age is less than 18. Additional information about these data can be obtained at http://www.meps.ahrq.gov.
Definitions
Children with special health care needs. Studying health care needs, access, utilization and expenditures for children with chronic conditions has always been difficult due to the low prevalence of most health conditions for children (Perrin, 2002; Bethel, Read, Stein, et al., 2002; Mangione-Smith, McGlynn, 1998). To address this problem, a standard definition of children with special health care needs (CSHCN) was developed (Bethel, Read, Stein, et al., 2002; McPherson, Arango, Fox, et al., 1998), and this definition was operationalized into a CSHCN screener questionnaire (Bethel, Read, Stein, et al., 2002). Starting in 2000, MEPS included the CSHCN screener as part of the Health Care Quality Enhancements that were added to its household survey to provide national estimates for the Agency for Healthcare Research and Qualitys congressionally mandated National Health Care Quality Report. In 2000, the CSHCN screener was included in a PAQ; for each child under 18 years of age in Panel 4/Round 4, and Panel 5/Round 2, parents were asked to complete a PAQ, a paper-and-pencil questionnaire. The CSHCN screener instrument consists of a series of question-sequences for each of five health domains (Bethel, Read, Stein, et al., 2002): the need or use of medicines prescribed by a doctor; the need or use of more medical care, mental health, or education services than is usual for most children; being limited or prevented in doing things most children can do; the need or use of special therapy, such as physical, occupational, or speech therapy; and the need or use of treatment or counseling for emotional, developmental, or behavioral problems. Parents who responded yes to any of the initial questions in the five question-sequences were then asked up to two follow-up questions about whether the health domain was attributable to a medical, behavioral, or other health condition lasting or expected to last at least 12 months. Children with positive responses to at least one of the five health domains along with all of the follow-up questions were identified as having a SHCN. Children with a no response for at least one question for each of the five question-sequences were considered not to have a SHCN. Those children whose special health care need status could not be determined (due to missing data for some of the questions) were coded as unknown SHCN status (3.4 percent of children in 2000).
In addition to the CSHCN screener, the PAQ contained health care quality measures of children that were taken from the health plan version of CAHPS, an AHRQ sponsored family of survey instruments designed to measure quality of care from the consumers perspective. Having the CSHCN screener as part of MEPS allows the analysis of associations for children with special health care needs according to any of the information collected by MEPS and facilitates comparisons of children with and without special health care needs. More information about MEPS can be obtained through the MEPS Web site (www.meps.ahrq.gov). More information about CAHPS can be obtained through the CAHPS Web site (http://www.cahps.ahrq.gov/default.asp) or on the AHRQ Web site (www.ahrq.gov).
Type of service. Utilization data are shown separately in five broad categories in this report (table 3): Ambulatory visits; emergency department visits; hospital inpatient discharges; dental visits; and prescription medicines.
- Ambulatory visits: This category includes visits to medical providers seen in office-
based settings or clinics and also for visits to both physicians and other medical providers seen in hospital outpatient departments. Expenses include payments to medical providers in office-based settings and for hospital outpatient departments includes payments for services covered under the basic facility charge and those for separately billed physician services.
- Emergency department visits: This category includes visits to medical providers seen in emergency rooms (except visits resulting in a hospital admission).
- Hospital inpatient discharges: Hospital admissions that did not involve an overnight stay are excluded.
- Dental visits: This category includes visits for any type of dental care provider, including general dentists, dental hygienists, dental technicians, dental surgeons, orthodontists, endodontists, and periodontists.
- Prescription medicines: This category includes all prescribed medications initially purchased or otherwise obtained during 2000, as well as any refills.
Expenditures. Expenditures in this report refer to what is actually paid for health care services. More specifically, in MEPS expenditures are defined as the sum of direct payments for care received, including out-of-pocket payments for care received and payments made by private insurance, Medicare, Medicaid, and other sources. Payments for over-the-counter drugs and alternative care services are not included in MEPS total expenditures. Indirect payments not related to specific medical events, such as Medicaid Disproportionate Share and Medicare Direct Medical Education subsidies, are also not included.
This definition of expenditures differs somewhat from that used in MEPS predecessor surveys, the 1987 National Medical Expenditure Survey and the 1977 National Medical Care Expenditure Survey, in which charges rather than payments were used to measure medical expenditures. Users who wish to compare the expenditure data presented in this report with data from the 1987 survey should consult Zuvekas and Cohen (2002).
Out-of-pocket expenditures. The out-of-pocket expenditure estimates (tables 58) represent the expenses borne by individuals or their families for health care for which they were not reimbursed by insurance or other sources of payment.
Age. The 2000 PAQ was administered during Panel 5/Round 2 and Panel 4/Round 4 in late 2000 for each child in MEPS under 18 years of age as of July 1, 2000. In this report, age is based on the childs age as of July 1, 2000 (AGEJUL01 variable in the MEPS HC-050).
Race/ethnicity. Classifications by race/ethnicity in this report are based on the following four race/ethnicity groups: Hispanic, black non-Hispanic, white non-Hispanic, and other non-Hispanic. Classification by race and ethnicity is based on information reported in MEPS for each family member. First, respondents were asked if the persons main national origin or ancestry was Puerto Rican; Cuban; Mexican, Mexican American, or Chicano; other Latin American; or other Spanish. All persons whose main national origin or ancestry was reported as one of these Hispanic groups, regardless of racial background, were classified as Hispanic. All other persons were classified according to their reported race. The other non-Hispanic category, though included in the totals, is not shown separately in the tables. An estimated 4 percent of children were reported to be in the other non-Hispanic category in 2000.
Region. Each MEPS child was classified as living in one of the following four regions as defined by the U.S. Census Bureau. The round-specific variable REGION42 was used for the analyses in this report.
- Northeast: Maine, New Hampshire, Vermont, Massachusetts, Rhode Island, Connecticut, New York, New Jersey, and Pennsylvania.
- Midwest: Ohio, Indiana, Illinois, Michigan, Wisconsin, Minnesota, Iowa, Missouri, North Dakota, South Dakota, Nebraska, and Kansas.
- South: Delaware, Maryland, District of Columbia, Virginia, North Carolina, South Carolina, Georgia, Florida, Kentucky, Tennessee, Alabama, Mississippi, Arkansas, Louisiana, Oklahoma, and Texas.
- West: Montana, Idaho, Wyoming, Colorado, New Mexico, Arizona, Utah, Nevada, Washington, Oregon, California, Alaska, and Hawaii.
Residence. The place of residence is classified as inside a metropolitan statistical area (MSA) or outside an MSA. The definition and titles of MSAs are established by the U.S. Office of Management and Budget with the advice of the Federal Committee on Metropolitan Statistical Areas. The round-specific variable MSA42 was used for the analyses in this report.
Family income. Each child was classified according to total 2000 income of his or her family. In this report, income is expressed in terms of poverty status, the ratio of the familys income to the Federal poverty thresholds that control for the size of the family and the age of the head of the family. The following classification was used:
- Poor/near poor: Children in families with income less than 125 percent of the poverty line, including those whose losses exceeded their earnings, resulting in negative income.
- Low income: Children in families with income from 125 percent to less than 200 percent of the poverty line.
- Middle income: Children in families with income from 200 percent to less than 400 percent of the poverty line.
- High income: Children in families with income at or over 400 percent of the poverty line.
In MEPS, personal income from each household member was summed to create family income. Potential income sources asked about in the survey interview include annual earnings from wages, salaries, bonuses, tips, and commissions; business and farm gains and losses; unemployment and Workers Compensation payments; interests and dividends; alimony, child support, and other private cash transfers; private pensions; individual retirement account (IRA) withdrawals; Social Security and Department of Veterans Affairs payments; Supplemental Security Income and cash welfare payments from public assistance; TANF (Temporary Assistance for Needy Families, formerly known as Aid to Families with Dependent Children or AFDC); gains or losses from estates, trusts, partnerships C corporations, rent, and royalties; and a small amount of other income.
Health insurance status. Children (under age 18) were classified into the following three insurance categories based on household responses to health insurance status questions administered during Rounds 13 for Panel 5 and Rounds 35 for Panel 4.
- Any private: Children who, at any time during the year, had insurance that provides coverage for hospital and physician care (other than Medicare, Medicaid, or other public hospital/physician coverage) are classified as having private insurance. Coverage by TRICARE (Armed Forcesrelated coverage) is also included as private health insurance. Insurance that provides coverage for a single service only, such as dental or vision coverage, is not included.
- Public only: Individuals are considered to have public coverage only if they met both of the following criteria: They were not covered by private insurance at any time during the year, and they were covered by one of the following public programs at any point during the yearMedicare, Medicaid, or other public hospital/physician coverage.
- Uninsured: The uninsured are defined as people not covered by Medicare, Medicaid, other public hospital/physician programs, TRICARE, or private hospital/physician insurance at any time during the entire year or period of eligibility for the survey. Individuals covered only by non-comprehensive State-specific programs (e.g., Maryland Kidney Disease Program, Colorado Child Health Plan) or private single-service plans (e.g., coverage for dental or vision care only, coverage for accidents or specific diseases) are not considered to be insured.
Health status. The respondents were asked to rate the health of each person in the family according to the following categories: excellent, very good, good, fair, and poor. For this report, the round-specific variable RTHLTH42 was used, and the fair and poor categories were combined because of small sample sizes.
Sample Design and Accuracy of Estimates
Each year, the MEPS Household Component (HC) sample is drawn from those households that completed the prior years National Health Interview Survey (NHIS). For example, households selected for participation in MEPS Panel 5 (beginning in 2000) completed interviews in the 1999 NHIS, the sample for MEPS Panel 4 (beginning in 1999) was drawn from the 1998 NHIS, and so on. Because NHIS is used as a sampling frame, the MEPS design is not only nationally representative of the civilian noninstitutionalized population, but also includes an oversampling of Hispanics and blacks. NHIS is conducted by the National Center for Health Statistics (NCHS),
Centers for Disease Control and Prevention.
MEPS collects data via an overlapping panel design. Each household completes five interview rounds of data collection over a period of two and a half years, providing data for two full calendar years. Data from Rounds 1, 2, and 3 provide information for the first year of estimation, and data from Rounds 3, 4, and 5 provide data for the second year of estimates. The data in this report identify children with SHCN based on information collected in the paper-and-pencil PAQ. The PAQ was administered during late 2000 to parents of children in Round 2 of Panel 5 and Round 4 of Panel 4 for children who were alive as of the interview date and who were under 18 years of age as of July 1, 2000. For analytical purposes, a single person-level weight variable, SQPQW00F, has been provided for use with data from the PAQ (as well as with data from the self-administered questionnaire that was administered to adults during Round 2/Panel 5, and Round 4/Panel 4). In analyzing PAQ data, the analyst should use the SQPQW00F weight and subset to cases where AGEJUL01 is between 0 and 17.
In all, there were 6,581 children with positive SQPQW00F weights, and they produced an estimate of 72,420,907 children under 18 years of age (an estimate of the civilian, noninstitutionalized children population as of December 31, 2000). The Panel 4/Round 4 conditional response rate for the SAQ was 96.3 percent. The Panel 5/Round 2 conditional response rate for the PAQ was 96.2 percent. The conditional response rate for the 2000 PAQ after combining both panels was 96.3 percent.
Tests of statistical significance were used to determine whether the differences between populations existed at specified levels of confidence or whether they occurred by chance. Differences were tested using z-scores having asymptotic normal properties at the 0.05 level of significance. Unless otherwise noted, only statistical differences between estimates are discussed in the text. However, it should be noted that each individual significance test was conducted at the 0.05 level, which does not control the error rate for all significance tests conducted simultaneously at the 0.05 level.
The statistics presented in this report are affected by both sampling error and sources of nonsampling error, which include nonresponse bias, respondent reporting errors (response errors), and data processing misspecifications. The nonsampling errors, such as response errors, are difficult to measure, but every effort is made to minimize such errors at each step of the MEPS operation. The sampling error, however, can be measured by the variance of the estimator. A Taylor-series approach in SUDAAN is used to produce appropriate standard errors for weighted estimates from MEPS with its complex sample design. Standard errors for the MEPS estimates in this report are shown in tables 13, and in tables 4A8A (corresponding to estimates in tables 48). The MEPS person-level estimation weight, SQPQW00F, includes nonresponse adjustments and poststratification adjustments to population estimates derived from the Current Population Survey based on cross-classification by region, MSA status, age, sex, and race/ethnicity.
Rounding
Estimated percentages and average and median number of events were rounded to the nearest 0.1 percent, while estimated average and median total and out-of-pocket expenditures were rounded to two decimal places. All standard errors were rounded to two decimal places.
Some of the estimates for subgroups presented in the tables will not add exactly to the overall estimated population total as a consequence of rounding.
MEPS Expenditures Methodology
Expenditure estimates in this report are based on the sum of total payments for medical events in 2000 reported in the MEPS Household Component (HC). The HC collected annual data on the use of and associated expenditures for office- and hospital-based care, emergency room services, home health care, dental services, prescription medicines, and vision aids and other medical equipment and services. In addition, the MEPS Medical Provider Component (MPC) collected expenditure data from a sample of medical and pharmaceutical providers that provided care and medicines to sample people in 2000. Expenditure data collected in the MPC are generally regarded as more accurate than comparable data collected in the HC and were used to improve the overall quality of MEPS expenditure data in this report. For a more detailed description of the MPC, see Machlin and Taylor (2000). For more information about MEPS expenditure methodology, see Ezzati-Rice, Kashihara, and Machlin (2004).
Comparisons with Other Data
Because of methodological differences, caution should be used when comparing these data with data from other sources. A range of results is frequently found among surveys due to differences in whether or not it was interviewer or self-administered, whether it was conducted in person, by telephone, by mail, or Internet, and due to differences in question wording, the sequencing of questions, and the placement of questions.
^top
Tables
| 1. Number of children and percentage with special health care needs for selected characteristics: United States, 2000 |
| 2. Number of children and percentage distribution by selected characteristics for children according to special health
care need status: United States, 2000 |
| 3. Percentage of children with selected medical care use according to special health care need status: United States, 2000 |
| 4. Percentage of children with expendituresa and average and median total expenditures according to special health
care need status: United States, 2000 |
| 4A. Standard errors for percentage of children with expendituresa and for average and median total expenditures according to special health care need status: United States, 2000 |
| 5. Percentage of children with out-of-pocket expendituresa and average and median out-of-pocket expenditures
according to special health care need status: United States, 2000 |
| 5A. Standard errors for percentage of children with out-of-pocket expendituresa and for average and median
out-of-pocket expenditures according to special health care need status: United States, 2000, |
| 6. Percentage distribution of annual out-of-pocket expenditures for child's health servicesa as a percentage of
family income for all children: United States, 2000 |
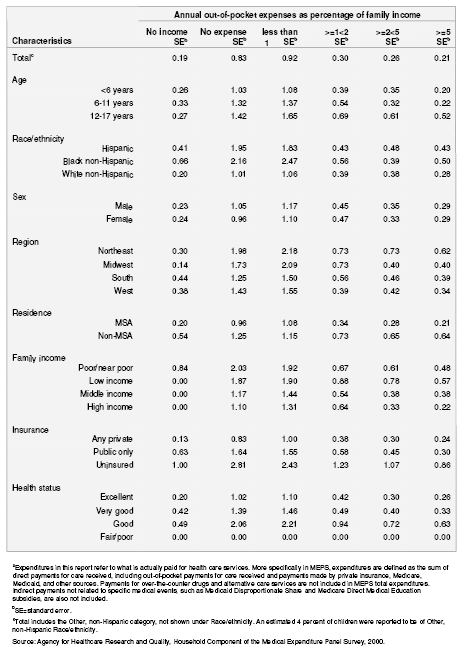
| 6A. Standard errors of percentage distribution of annual out-of-pocket expenditures for child's health servicesa as
a percentage of family income for all children: United States, 2000 |
| 7. Percentage distribution of annual out-of-pocket expenditures for child's health servicesa as a percentage of
family income for children with special health care needs: United States, 2000 |
| 7A. Standard errors of percentage distribution of annual out-of-pocket expenditures for child's health servicesa as a
percentage of family income for children with special health care needs: United States, 2000 |
| 8. Percentage distribution of annual out-of-pocket expenditures for child's health servicesa as a percentage of family
income for children without special health care needs: United States, 2000 |
| 8A. Standard errors of percentage distribution of annual out-of-pocket expenditures for child's health servicesa as a
percentage of family income for children without special health care needs: United States, 2000 |
Table 1. Number of children and percentage with special health care needs for selected characteristics: United States, 2000
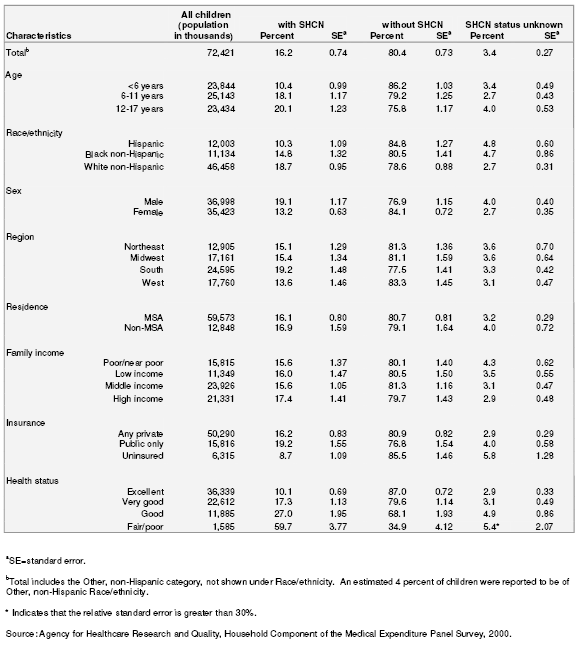
Table 2. Number of children and percentage distribution by selected characteristics for children according to special health care need status: United States, 2000
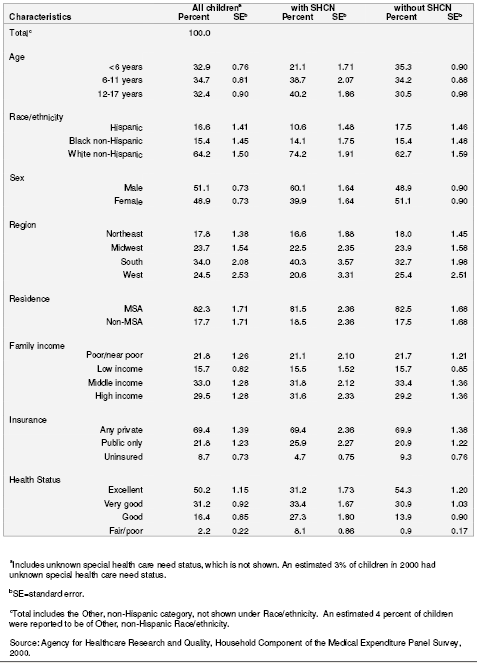
Table 3. Percentage of children with selected medical care use according to special health care need status: United States, 2000
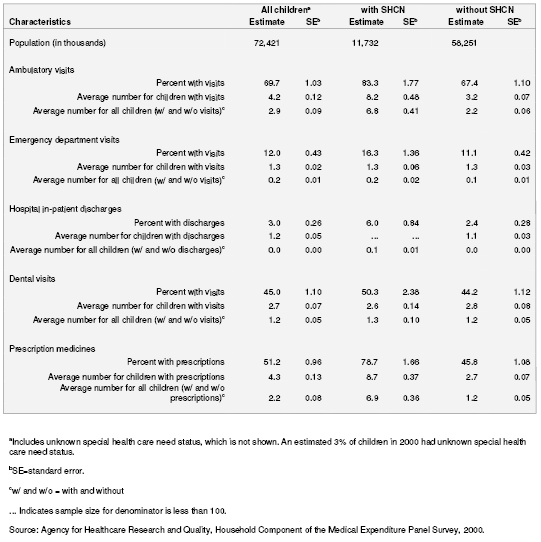
Table 4. Percentage of children with expendituresa and average and median total expenditures according to special health care need status: United States, 2000
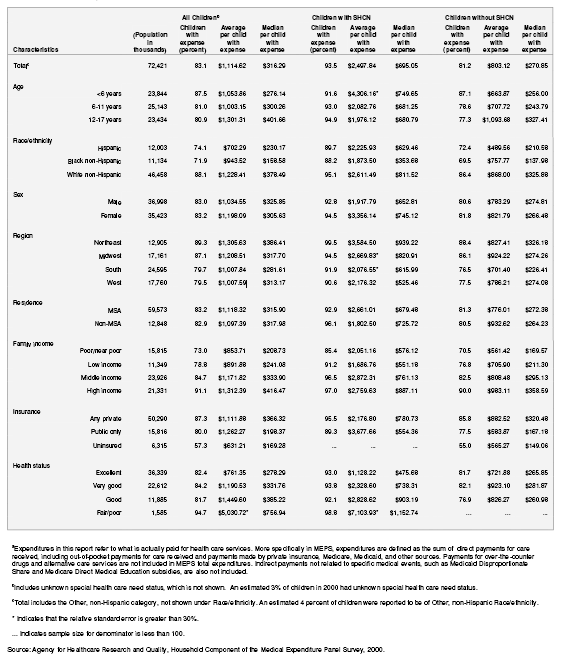
Table 4A. Standard errors for percentage of children with expendituresa and for average and median total expenditures according to special health care need status: United States, 2000
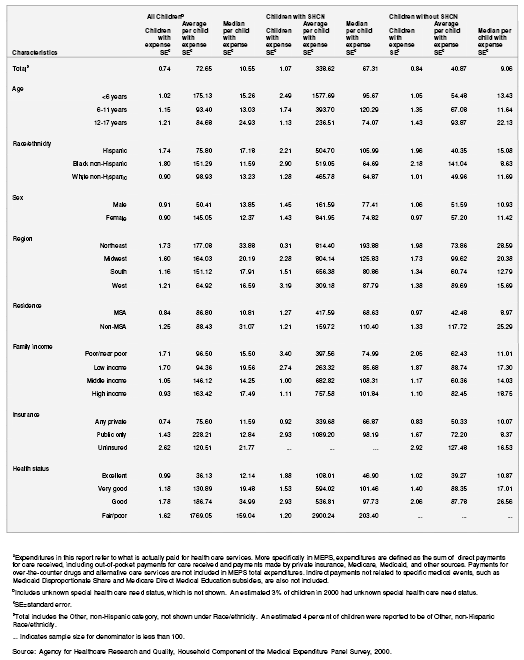
Table 5. Percentage of children with out-of-pocket expendituresa and average and median out-of-pocket expenditures according to special health care need status: United States, 2000
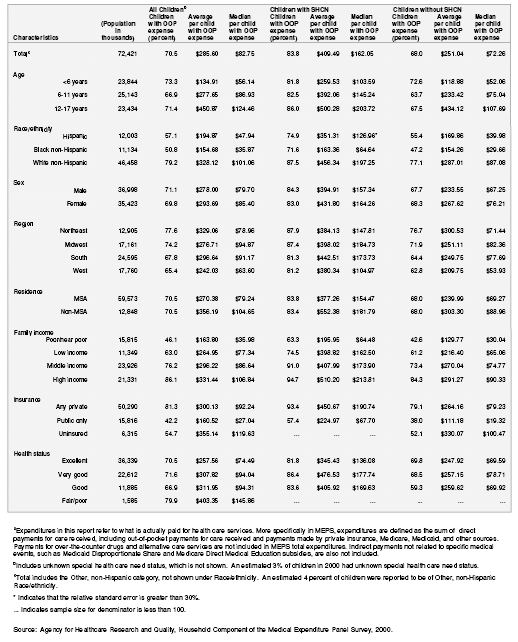
Table 5A. Standard errors for percentage of children with out-of-pocket expendituresa and for average and median out-of-pocket expenditures according to special health care need status: United States, 2000
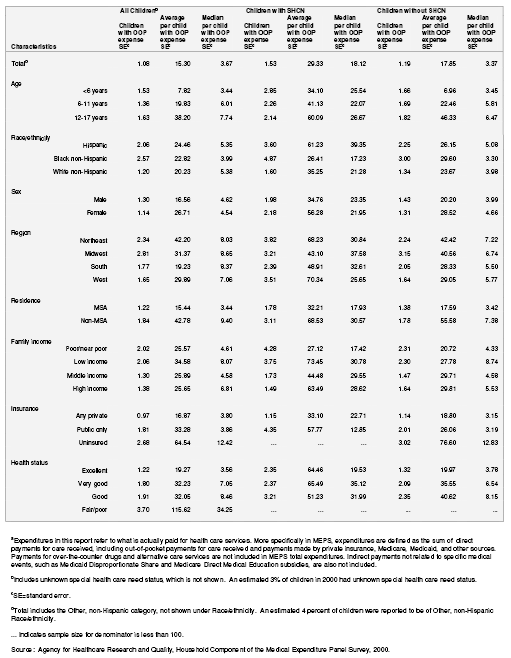
Table 6. Percentage distribution of annual out-of-pocket expenditures for child's health servicesa as a percentage of family income for all children: United States, 2000
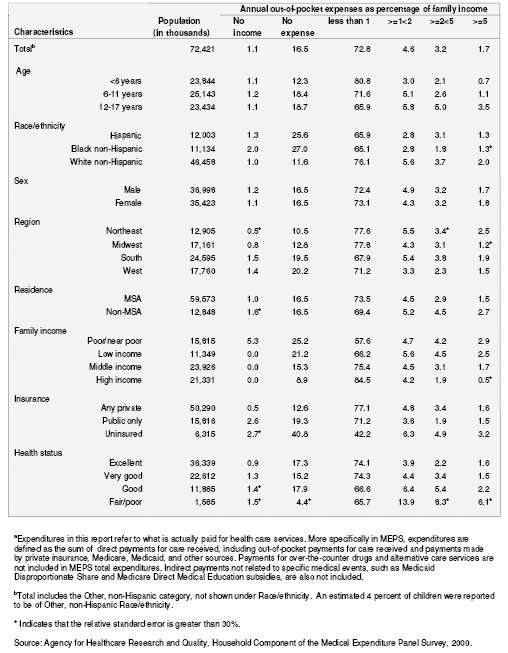
Table 6A. Standard errors of percentage distribution of annual out-of-pocket expenditures for child's health servicesa as a percentage of family income for all children: United States, 2000
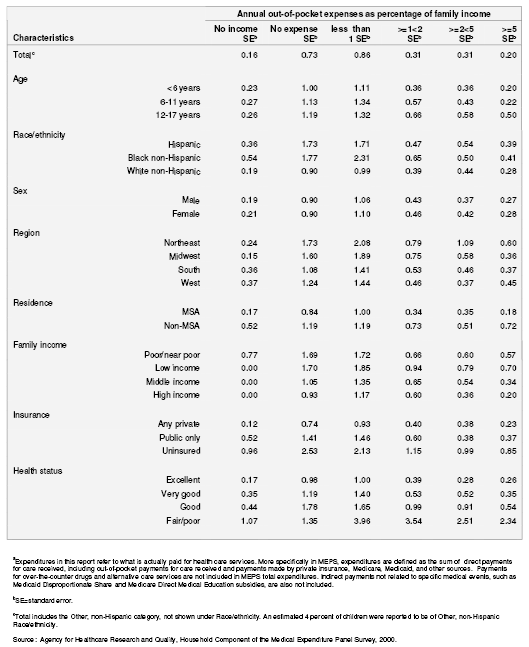
Table 7. Percentage distribution of annual out-of-pocket expenditures for child's health servicesa as a percentage of family income for children with special health care needs: United States, 2000
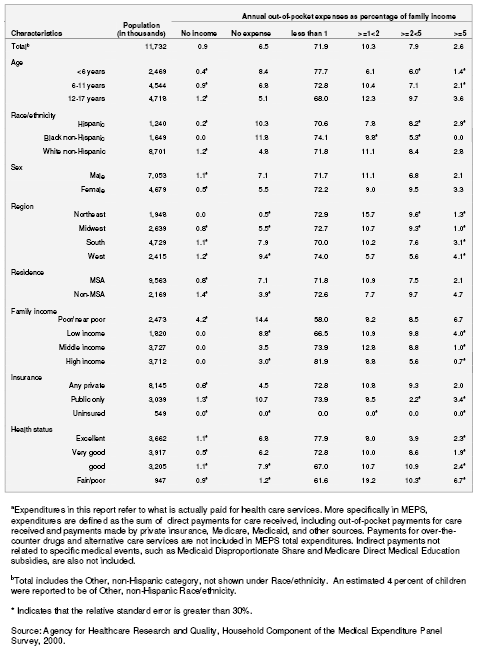
Table 7A. Standard errors of percentage distribution of annual out-of-pocket expenditures for child's health servicesa as a percentage of family income for children with special health care needs: United States, 2000
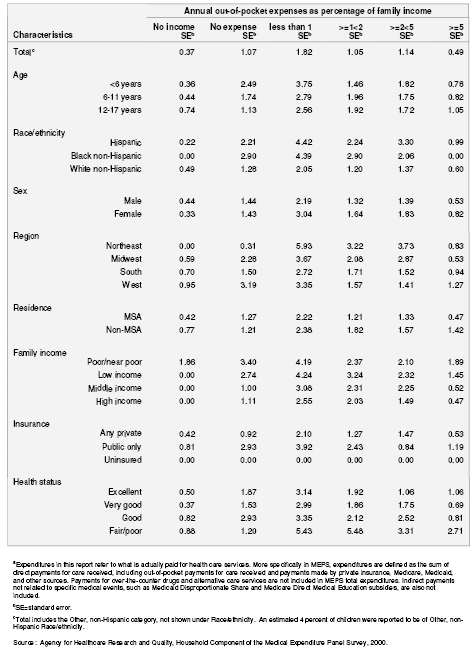
Table 8. Percentage distribution of annual out-of-pocket expenditures for child's health servicesa as a percentage of family income for children without special health care needs: United States, 2000
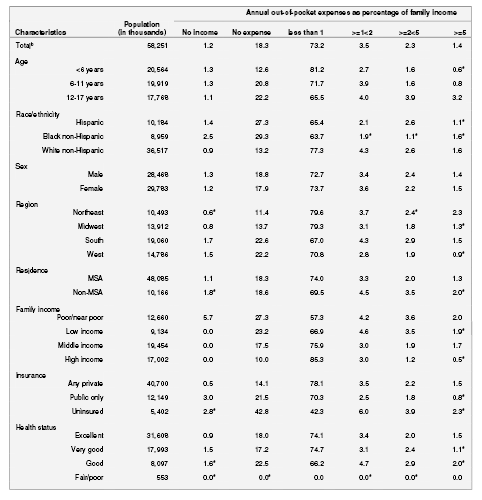
Table 8a. Standard errors of percentage distribution of annual out-of-pocket expenditures for child's health servicesa as a percentage of family income for children without special health care needs: United States, 2000
^top
Suggested
Citation: Research Findings #24: Utilization and Expenditures for Children with Special Health Care Needs. January 2006. Agency
for Healthcare Research and Quality, Rockville,
MD.
http://www.meps.ahrq.gov/data_files/publications/rf24.shtml |
|
