Research
Findings #7: Use of Health Care Services, 1996
Nancy A. Krauss, M.S., Steven Machlin, M.S.,
and Barbara L. Kass, M.P.H., C.H.E.S., Agency for Health Care Policy
and Research
Examining variations in the use of health
care services is an important means for evaluating the adequacy
of access to care across the population. Underutilization
of health care services can be the result of limited access
to care because of the lack of adequate health insurance or
financial resources, or limited availability of services in
certain areas. Comparing patterns of use by subpopulations
presumed to require more care--such as the elderly, those
in poor health, or the terminally ill--with the general population
is one way of determining whether those most in need of care
actually receive it.
This report describes
several aspects of health care use in the United States
during calendar year
1996, including the proportion of people receiving ambulatory
medical care in office-based and hospital-based settings,
dental care, inpatient hospital stays, home health services,
and prescription medicines. Specific comparisons are made
by age, sex, race/ethnicity, perceived health status, health
insurance coverage, usual source of care, and metropolitan
vs. nonmetropolitan residence. Separate estimates also are
reported for children’s use of ambulatory medical and
dental services.
The health care use estimates presented
in this report are for the civilian noninstitutionalized population
of the United States during calendar year 1996. The estimates
are derived from data provided by household respondents in
the 1996 Medical Expenditure Panel Survey (MEPS) Household
Component (HC). A technical appendix at the end of this report
provides detailed descriptions of the MEPS HC, including data
collection methods, data editing, sample size, and statistical
procedures used for deriving estimates.
^top
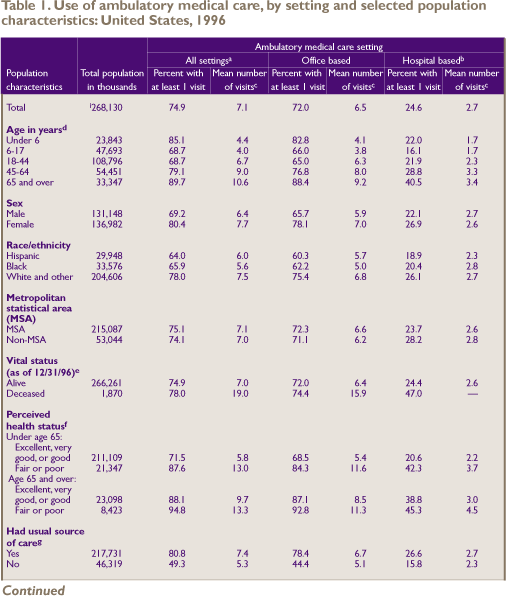
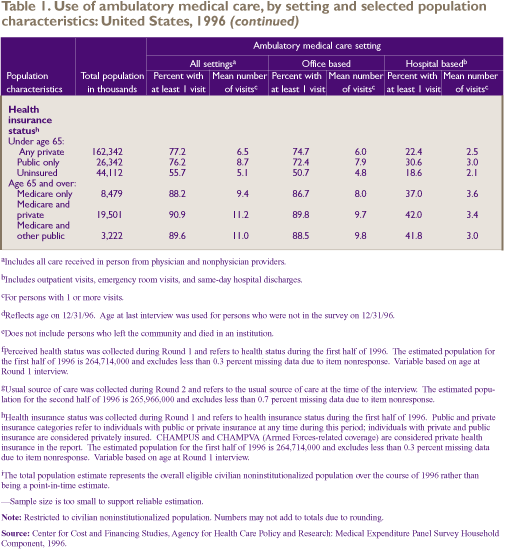
During 1996, three-quarters (74.9 percent)
of the U.S. civilian noninstitutionalized population received
ambulatory care from at least one medical provider (physician
or nonphysician) in an office-based or hospital-based setting
(Table 1). For people using these services, the mean number
of visits per person was 7.1, while the median number of visits
(not shown in table) was 4.0. While 72.0 percent of Americans
visited an office-based setting, only one-quarter (24.6 percent)
of the population received ambulatory hospital-based services,
which include visits to hospital outpatient clinics, emergency
room visits, and hospital admissions that did not result in
an overnight stay. The mean number of office-based visits
(6.5) was more than twice as large as the mean number of hospital-based
visits (2.7) for people with those types of ambulatory visits.
Approximately 21.7 percent of people received care in both
hospital-based and office-based settings (not shown in table).
Types of Office-Based Providers
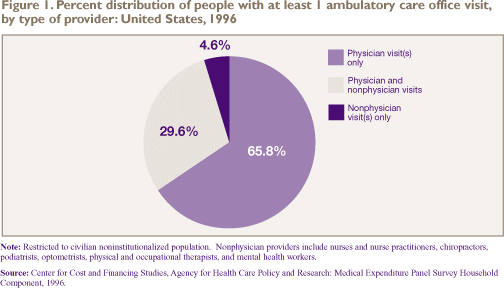
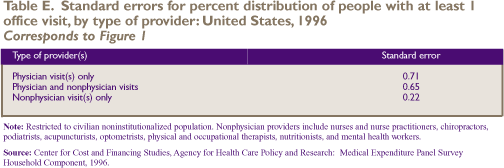
Figure 1 displays the types of health care
providers who gave care to the 72.0 percent of the population
who had at least one office-based visit. Of this group, most
people (95.4 percent) received medical care from a physician:
65.8 percent received care from physician providers only and
29.6 percent received care from both physicians and nonphysician
providers. Only 4.6 percent received health care exclusively
from nonphysician providers, which include nurses and nurse
practitioners, physical and occupational therapists, podiatrists,
optometrists, chiropractors, and mental health workers.
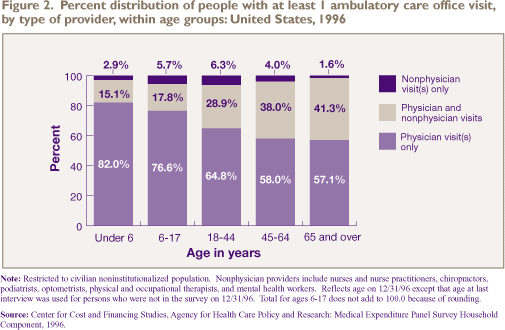
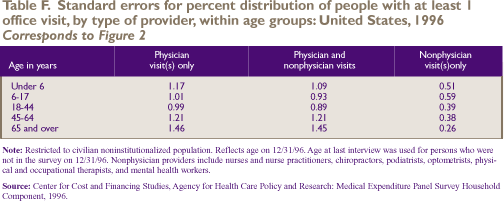
The type of provider seen varies dramatically
by age (Figure 2). The percent of people who saw medical doctors
for all their visits decreased with age, from 82.0 percent
for children under age 6 to 57.1 percent for people age 65
and over. In contrast, the percent of people who saw physicians
in some visits and nonphysicians in other visits rose from
15.1 percent for young children to about 41.3 percent for
the elderly population. The proportion of people who saw only
nonphysician providers was small in all age groups (6.3 percent
or less).
Demographic Characteristics
As shown in Table 1, children under age
6 and persons age 65 and over were the most likely to have
received ambulatory care (85.1 percent and 89.7 percent, respectively)
in 1996. Among those who used ambulatory care, older age groups
(45-64 and 65 and over) had more ambulatory visits than younger
people, regardless of the setting.
Overall, men were less likely than women
to have received any ambulatory medical services (69.2 percent
and 80.4 percent, respectively). This trend is observed for
both office-based and hospital-based settings. Among those
who received ambulatory care, there was no difference in the
mean number of visits for men and women in hospital-based
settings, but women averaged about one more visit than men
in office-based settings.
Use of ambulatory care was significantly
lower among blacks and Hispanics (65.9 percent and 64.0 percent,
respectively) compared with the group of whites and people
of other racial/ethnic backgrounds (78.0 percent). Furthermore,
among those who received any ambulatory care in 1996, the
mean number of visits also was higher for the group of whites
and others (7.5) than for blacks (5.6) and Hispanics (6.0).
People in the white and other group were more likely than
blacks or Hispanics to have received either office-based or
hospital-based medical care, but smaller racial/ethnic differences
were observed in hospital-based settings.
Other Characteristics
Health care use estimates for the approximately
1.9 million civilian noninstitutionalized persons who died
during calendar year 1996 are included in Table 1. Indicative
of higher health care use rates during the last months of
life, the mean number of ambulatory visits for people who
died is about 21/2 times higher than for the rest of the population
(19.0 visits compared with 7.0 visits for people who had at
least one visit). Although people who died in 1996 were just
as likely as the rest of the population to have used office-based
services, they were almost twice as likely to have had at
least one hospital-based visit (47.0 percent) compared with
the rest of the population (24.4 percent).
Higher ambulatory medical care use, both
in terms of the likelihood of use and the number of visits,
was associated with fair or poor health for both the elderly
and the non-elderly (Table 1). Elderly people in fair or poor
health were significantly more likely to use ambulatory care
than any other age group, regardless of health status.
Having a usual source of care also was associated
with higher use. People without a usual source of care were
less likely to have had any ambulatory medical care in 1996,
regardless of the type of setting. The mean number of visits
to office-based providers also was significantly lower for
people lacking a usual source of care (5.1 visits) than for
those who reported a usual source of care (6.7 visits). Having
a usual source of care also increased the likelihood of using
hospital-based services (26.6 percent, compared with 15.8
percent for those without a usual source of care) but had
no relationship to the number of hospital-based visits.
Overall, people under
age 65 who had public or private health insurance coverage
during the first half
of 1996 were more likely than their uninsured counterparts
to use ambulatory medical services. Among people under 65
who reported at least one ambulatory visit, those covered
only by public insurance had significantly more ambulatory
visits (8.7) than either the uninsured (5.1) or persons with
private coverage (6.5). For elderly people, having coverage
in addition to Medicare was not associated with differences
in the use of ambulatory services.
^top
In 1996, approximately 115 million Americans,
or 43.2 percent of the population (not shown in table), received
dental care. (Dental care includes visits to general dentists,
dental hygienists, dental technicians, endodontists, orthodontists,
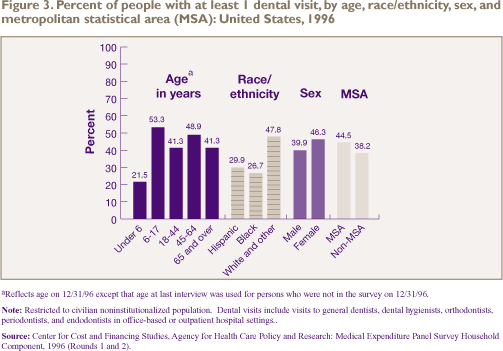
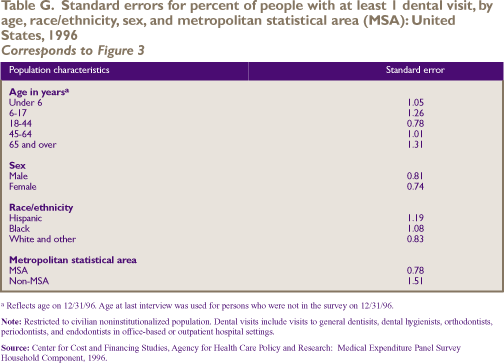
and periodontists.) Figure 3 shows the proportion of people
who had at least one dental visit by selected demographic
characteristics. Children ages 6-17 were more likely than
any other age group to have had a dental visit. Men were less
likely than women to have received any dental care in 1996
(39.9 percent and 46.3 percent, respectively). Blacks (26.7
percent) and Hispanics (29.9 percent) were less likely than
whites and others (47.8 percent) to have received dental care
in 1996. People not living in metropolitan statistical areas
(MSAs) were less likely than those who did live in MSAs to
receive dental care.
^top
Use of health
care services is critical not only for children’s health,
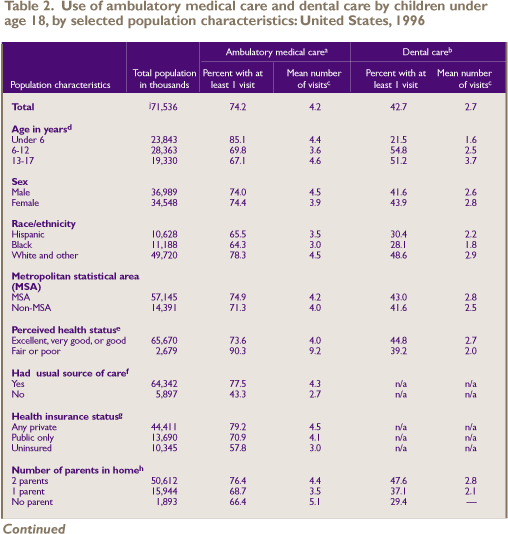
but for their overall well-being and development. Table
2 shows the use of ambulatory
medical and dental care by selected demographic, health, and
family characteristics for children under age 18.
Ambulatory Medical Care
Approximately three-quarters (74.2 percent)
of children under age 18 received ambulatory medical care
in 1996, averaging a mean number of 4.2 visits for children
with at least one visit. The median number of visits for children
with at least one visit was 2.0 (not shown in table). Children
under 6 (85.1 percent) were more likely than children ages
6-12 (69.8 percent) or 13-17 (67.1 percent) to have seen a
medical provider in an ambulatory setting. Although boys and
girls were equally likely to have received ambulatory medical
services, boys had a higher average number of visits (4.5,
compared to 3.9 for girls). Children in the white and other
group were more likely to have had at least one provider visit
in 1996 (78.3 percent) compared with either black children
(64.3 percent) or Hispanic children (65.5 percent). Furthermore,
among those who did receive ambulatory care, blacks and Hispanics
averaged fewer visits (3.0 and 3.5, respectively) than children
who were classified as white and other (4.5). Children living
in MSAs were about as likely as their counterparts outside
MSAs to have received ambulatory services during 1996 (74.9
percent and 71.3 percent, respectively).
Perceived health status
was associated with both the likelihood of receiving any care
and the number of
provider visits. Most children(90.3 percent) reported as
being in fair or poor health received at least one provider
visit during 1996, significantly more than the percent for
children reported as being in excellent, very good, or good
health (73.6 percent). Children in fair or poor health averaged
5.2 more ambulatory provider visits than children in excellent,
very good, or good health.
Having a usual source of care was associated
with a nearly twofold increase in the likelihood that a child
received some ambulatory medical services in 1996 (77.5 percent
versus 43.3 percent). Furthermore, children with a usual source
of care had a mean of 1.6 more visits than children lacking
a usual source of care (4.3 versus 2.7).
Like the general population, children with
public and private health insurance coverage made more use
of ambulatory services--both in terms of the likelihood of
use and the number of visits--than uninsured children. Among
children with at least one visit, having two parents in the
home is associated with a higher average number of visits,
but children living with neither parent were likely to have
more visits on average (5.1) than children living either with
both parents (4.4) or one parent (3.5).
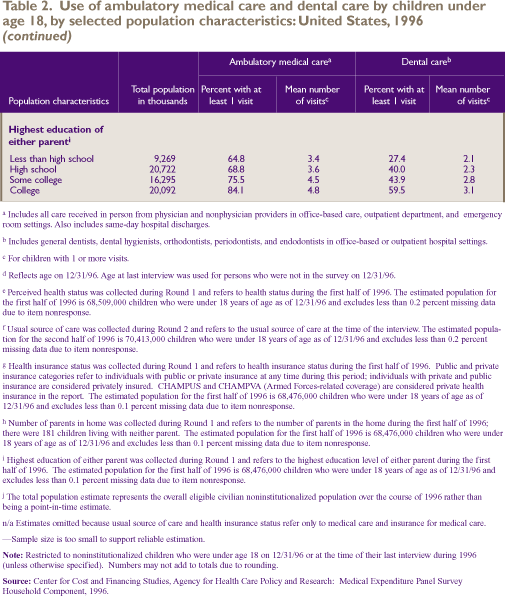
The level of
parents education was significantly associated with children’s
ambulatory care use. In general, a higher level of parental
education was associated with an
increased likelihood that a child had at least one ambulatory
visit in 1996. Moreover, children living in a household where
neither parent attended at least some college had significantly
fewer provider visits than children living in a household
where at least one parent attended or completed college.
Dental Care
Table 2 shows that, overall, only 42.7 percent
of children under age 18 received dental care in 1996. However,
about half of children ages 6-12 (54.8 percent) and ages 13-17
(51.2 percent) had at least one dental visit. Children under
age 6 were the least likely (only 21.5 percent) to receive
dental care. For those receiving any dental care, older children
(ages 13-17) averaged 1.2 visits more than children ages 6-12
and 2.1 visits more than the youngest age group (under 6).
This differential is likely attributable to more orthodontic
visits among children ages 13-17. Dental care use was not
different for boys than for girls, nor were any differences
noted by place of residence (MSA versus non-MSA). Children
grouped as white and other were more likely than either black
or Hispanic children to have had a dental visit: 48.6 percent
for the white and other group, compared with 28.1 percent
for blacks and 30.4 percent for Hispanics. Children in good
health and those in poor health were about equally likely
to have received any dental care (44.8 percent and 39.2 percent,
respectively). However, of those who had a visit, children
in good health averaged more visits (2.7) than children in
poor health (2.0).
Children living
with both parents were more likely to have had dental care
(47.6 percent) than children
living with only one parent (37.1 percent) or children living
with neither parent (29.4 percent). As with children’s
ambulatory medical care, increases in parents’ education
were associated with an increase in the likelihood of receiving
dental services. Therefore, children living in a household
with a parent who had completed college were almost twice
as likely to see a dental provider as those living in a household
where neither parent hadcompleted high school (59.5 percent
and 27.4 percent, respectively).
^top
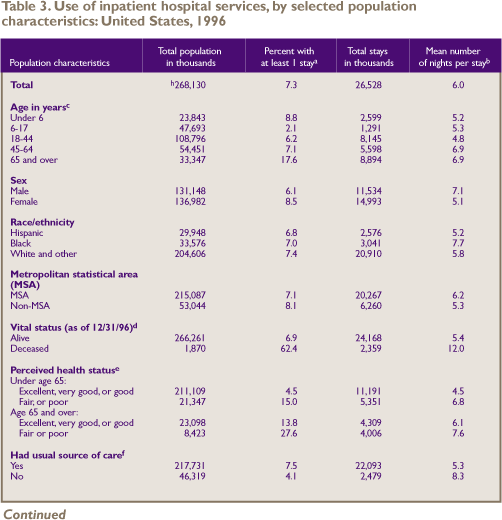
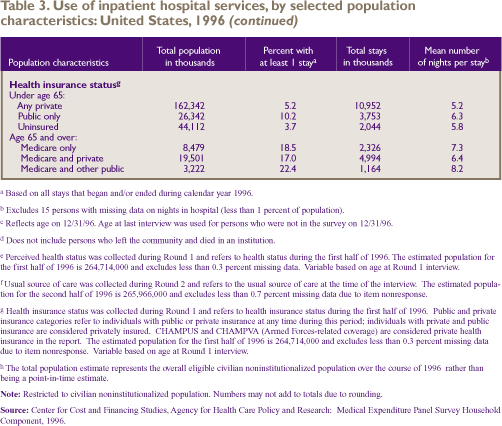
Table 3 shows that 7.3 percent of the total
population (approximately 19.6 million Americans) had at least
one inpatient hospital stay during calendar year 1996. The
mean number of nights spent in the hospital per stay was 6.0.
The likelihood of an inpatient stay was lowest for children
ages 6-17 (2.1 percent) and highest for people age 65 and
over (17.6 percent). Among those who had an inpatient stay,
people age 45 and over averaged 6.9 nights per stay, significantly
higher than children under age 18, who averaged about 5 nights
per stay.
While women (8.5 percent) were more likely
than men (6.1 percent) to have at least one overnight hospital
stay, stays for men were about 2 nights longer, on average,
than those for women: 7.1 nights per stay for men compared
with 5.1 nights per stay for women.
There were no observed
racial/ethnic differences regarding the likelihood of a
hospital stay, but blacks averaged more nights per stay (7.7)
than
Hispanics (5.2). Nearly two-thirds (62.4 percent) of people
who died during calendar year 1996 had a hospitalization during
the year, a substantially higher proportion than for the rest
of the population (6.9 percent). Moreover, people who died
in 1996 spent about twice as many nights in the hospital per
stay (12.0) as the rest of the population (5.4).
Poor health increased the likelihood of
an inpatient stay as well as the average number of nights
per stay for both the elderly and the non-elderly population.
Having a usual source of care was also associated with a higher
likelihood of an inpatient stay during 1996 (7.5 percent,
compared with 4.1 percent for those lacking a usual source
of care).
For the population under age 65, people
covered only by public insurance were almost twice as likely
(10.2 percent) as those with private health insurance (5.2
percent) and 2 1/2 times as likely as the uninsured population
(3.7 percent) to have had a hospital stay. There were no significant
differences in the mean number of nights per stay by type
of insurance coverage for people who had a hospital stay.
Similarly, people age 65 and over who had
other public insurance coverage in addition to Medicare were
more likely to have had a hospital stay than elderly people
with only Medicare or Medicare and private insurance. However,
for people with at least one stay, having insurance in addition
to Medicare was not associated with significant differences
in the mean number of nights per stay.
Elderly people with Medicare and private
insurance were less likely to have an inpatient stay (17.0
percent) and averaged fewer nights in the hospital per stay
(6.4 nights) than those with Medicare and other public insurance:
22.4 percent of the latter group had at least one hospital
stay and averaged 8.2 nights per stay.
^top
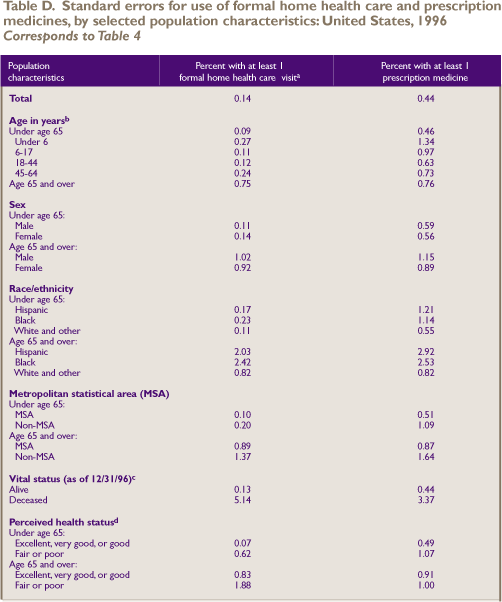
During 1996, 2.7 percent of the population,
approximately 7.2 million Americans, received home health
care provided by hospitals, home health agencies, nursing
homes, or self-employed individuals (Table 4).
Approximately 13.8 percent of the elderly
population received home health care, substantially more than
any other age group. Among the elderly, 16.0 percent of women
received home health services, significantly more than men
(10.9 percent). For both the elderly and non-elderly, racial/ethnic
differences were not significant. There were no observed differences
in home health care use by place of residence among younger
people, but elderly people not residing in MSAs were more
likely to receive home health care (16.6 percent) than those
living in MSAs (13.0 percent).
The likelihood of receiving home health
care was substantially higher for those who died during calendar
year 1996. Of people who died, 41.0 percent had received home
health care, compared with only 2.4 percent of the rest of
the population. This difference may reflect in part the use
of home hospice services (Haupt, 1998).
For both the elderly and non-elderly, those
in poor health were more likely than people in good health
to receive home health care services. Home health care services
also were more likely to be used by people with a usual source
of care (2.8 percent) than those without a usual source of
care (0.9 percent). Among the elderly, people with other public
health insurance coverage in addition to Medicare were more
than twice as likely to receive home health care (29.5 percent)
as people with Medicare only (13.9 percent) or Medicare and
private insurance (12.1 percent).
^top
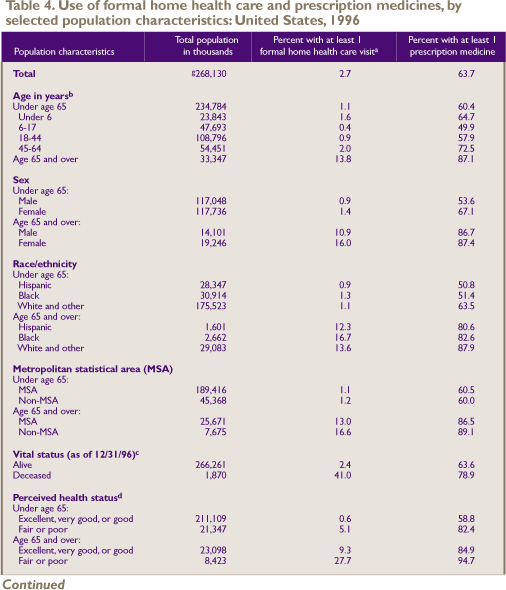
Table 4 also shows that nearly two-thirds
of the population (63.7 percent) obtained at least one prescription
medicine in 1996. Children under age 6 were more likely to
have obtained a prescription medicine (64.7 percent) than
older children (49.9 percent). The vast majority (87.1 percent)
of elderly people obtained at least one prescription medicine,
significantly more than any other age group. In the under-65
group, women were more likely than men to have obtained a
prescription medicine (67.1 percent compared with 53.6 percent),
but no such difference was observed among the elderly population.
Both elderly and non-elderly people grouped
as whites and others were more likely than blacks or Hispanics
to have obtained a prescription medicine. Although statistically
significant, racial/ethnic differences were not as large among
elderly persons.
Overall, vital status and perceived health
were related to whether or not an individual obtained a prescription
medicine. People who died during 1996 were more likely to
have obtained a prescription medicine than the rest of the
population. Moreover, both elderly and non-elderly people
in poor health were more likely than those in good health
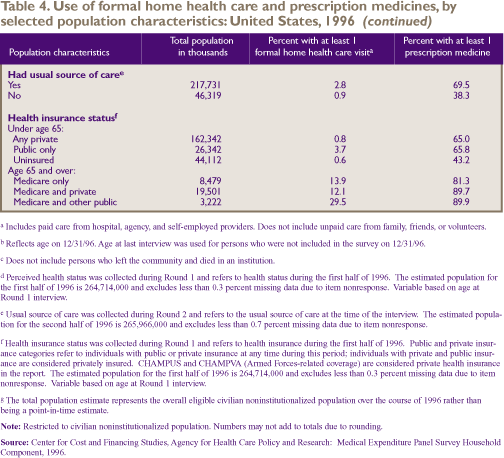
to have obtained a prescription medicine. Having a usual source
of care was also significantly associated with the likelihood
of obtaining at least one prescription medicine in 1996 (69.5
percent versus 38.3 percent).
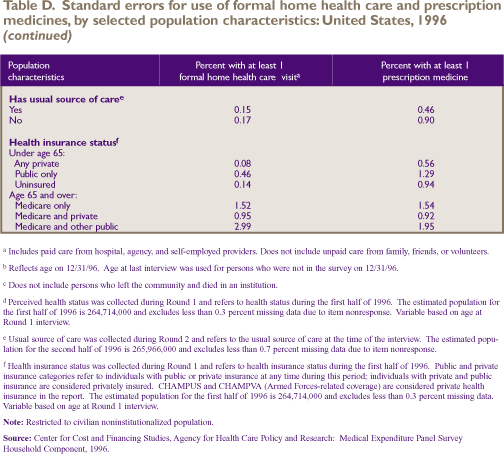
Uninsured people under age 65 were less
likely to have obtained a prescription medicine (43.2 percent)
than people with either private insurance (65.0 percent) or
public insurance (65.8 percent). Elderly people who were covered
by Medicare only were less likely to have obtained a prescription
medicine (81.3 percent) than those with Medicare and private
insurance (89.7 percent) or Medicare and other public insurance
(89.9 percent).
^top
Data from the 1996 MEPS HC indicate that
about three-quarters of the U.S. civilian noninstitutionalized
population received ambulatory care from a medical provider
in 1996. The highest use of ambulatory medical care was observed
among people who died in 1996, children under age 6, the elderly,
and those in poor health. Having a usual source of care was
also associated with high use of ambulatory services. This
difference was particularly dramatic for children: 77.5 percent
of children with a usual source of care had at least one ambulatory
visit, compared with 43.3 percent of children lacking a usual
source of care.
Overall, people under age 65 with either
public or private insurance coverage were more likely to receive
ambulatory care than their uninsured counterparts. Having
coverage in addition to Medicare was not associated with differences
in the use of ambulatory services among the elderly. Data
from this report also indicate that the elderly were more
likely than younger age groups to use the ambulatory services
of nonphysician providers.
Only 42.7 percent of the population (approximately
116 million Americans) received dental care in 1996. Children
ages 6-17 were the most likely to have had at least one dental
visit.
Approximately 7.3 percent of the American
population had at least one inpatient hospital stay. Poor
health increased the likelihood of an inpatient stay, regardless
of age. Moreover, people who died during 1996 were substantially
more likely than the rest of the population to have had a
hospital stay. Decedents also spent about twice as many nights
in the hospital per stay than the rest of the population (12.0
nights per stay compared with 5.4). Among the population under
age 65, people with public insurance were significantly more
likely to have had a hospital stay than either people with
private insurance or the uninsured. Similarly, elderly people
who had other public insurance coverage in addition to Medicare
were more likely to have had a hospital stay than those with
only Medicare or with Medicare and private insurance. No racial/ethnic
differences were observed regarding the likelihood of having
a hospital stay in 1996.
About 7.2 million Americans (2.7 percent
of the population) received home health care during calendar
year 1996. Compared with the younger population, the elderly
were more likely to have had a home health visit. Furthermore,
elderly people with other public health insurance coverage
in addition to Medicare were more than twice as likely to
have had a home health visit in 1996 (29.5 percent) than those
with Medicare only (13.9 percent) or Medicare and private
insurance (12.1 percent). More than a third (41.0 percent)
of people who died during the year received some formal home
health care.
Nearly two-thirds (63.7 percent) of the
population obtained at least one prescription medicine in
1996. The elderly and people in poor health were more likely
to obtain a prescription than younger people and those in
good health. For the younger population, being uninsured reduced
the likelihood of obtaining a prescription medicine. Elderly
people were more likely to obtain a prescription medicine
if they were covered by either private or other public insurance
in addition to Medicare.
^top
Figures
 ^top
Tables
^top
Cohen J. Design and methods of the Medical
Expenditure Panel Survey Household Component. Rockville (MD):
Agency for Health Care Policy and Research; 1997. MEPS Methodology
Report No. 1. AHRQ Pub. No. 97-0026.
Cohen JW, Monheit AC, Beauregard KM, et
al. The Medical Expenditure Panel Survey: a national health
information resource. Inquiry 1996;33:373-89.
Cohen S. Sample design of the 1996 Medical
Expenditure Panel Survey Household Component. Rockville (MD):
Agency for Health Care Policy and Research; 1997. MEPS Methodology
Report No. 2. AHRQ Pub. No. 97-0027.
Haupt BJ. Characteristics of hospice care
users: data from the 1996 National Home and Hospice Care Survey.
Hyattsville (MD): National Center for Health Statistics; 1998.
Advance Data From Vital and Health Statistics, No. 299. DHHS
Pub. No. (PHS) 98-1250.
Vistnes JP, Monheit AC. Health insurance
status of the U.S. civilian noninstitutionalized population:
1996. Rockville (MD): Agency for Health Care Policy and Research;
1997. MEPS Research Findings No. 1. AHRQ Pub. No. 97-0030.
^top
Appendix
The data in this report were obtained in
the first three rounds of interviews for the Household Component
(HC) of the 1996 Medical Expenditure Panel Survey (MEPS).
MEPS is cosponsored by the Agency for Health Care Research
and Quality (AHRQ) and the National Center for Health Statistics
(NCHS). The MEPS HC is a nationally representative survey
of the U.S. civilian noninstitutionalized population that
collects medical expenditure data at both the person and household
levels. The focus of the MEPS HC is to collect detailed data
on demographic characteristics, health conditions, health
status, use of medical care services, charges and payments,
access to care, health insurance coverage, income, and employment.
In other components of MEPS, data are collected on the use,
charges, and payments reported by providers, residents of
licensed or certified nursing homes, and the supply side of
the insurance market.
The sample for the
MEPS HC was selected from respondents to the 1995 National
Health Interview Survey
(NHIS), which was conducted by NCHS. NHIS provides a nationally
representative sample of the U.S. civilian noninstitutionalized
population and reflects an oversampling of Hispanics and blacks.
The MEPS HC collects data through an overlapping panel design.
In this design, data are collected through a precontact interview
that is followed by a series of five rounds of interviews
over a period of 2 1/2 years. Interviews are conducted with
one member of each family, who reports on the health care
experiences of the entire family. Two calendar years of medical
expenditure and utilization data are collected in each household
and captured using computer-assisted personal interviewing
(CAPI). This series of data collection rounds is launched
again each subsequent year on a new sample of households to
provide overlapping samples of survey data that will provide
continuous and current estimates of health care expenditures.
The reference period for Round 1 of the MEPS HC was from January
1, 1996, to the date of the first interview, which occurred
during the period from March through August 1996. The reference
period for Round 2 of the MEPS HC was from the date of the
first interview (March-August 1996) to the date of the second
interview, which took place during the period from August
through December 1996. The reference period for Round 3 was
from the date of the second interview (August-December 1996)
to the date of the third interview, which occurred during
the period from February through July 1997. Estimates in this
report are based on characteristics as of December 31, 1996,
or the last date that the sample person was part of the civilian
noninstitutionalized population living in the United States
prior to December 31, 1996.
The utilization variables used to derive
estimates for this report are based on the number of visits
for health care that were reported as occurring in calendar
year 1996 during the first three rounds of interviews. Utilization
events for sampled persons are classified as office-based
visits, ambulatory hospital-based visits, inpatient hospital
stays, dental visits, home health visits, and obtaining prescription
medicine. Minimal data editing was done on health care utilization
variables.
Unless otherwise specified,
the utilization estimates are based on 21,571 sample persons
who were in the
U.S. civilian noninstitutionalized population for part or
all of calendar year 1996. Examples of persons with part-year
information include newborns, persons who died during the
year, and those who resided in an institution or were in the
military for part of the year. Utilization was measured for
deceased persons for the period between January 1 and the
date of death, while utilization for newborns was measured
from the date of birth to December 31. Utilization that occurred
during periods of full-time active-duty military service or
while residing in an institution was not included. The 21,571
sample persons were used to develop population estimates for
a total of 268,130,477 persons who were in the U.S. civilian
noninstitutionalized population for part or all of 1996.
Ambulatory Office-Based Events
Office-based events include visits to physician
and nonphysician providers as well as office-based providers
of unknown type. Telephone contact with office-based providers,
regardless of provider type, is not included in the estimates.
Examples of nonphysician providers include chiropractors,
physical and occupational therapists, nurses and nurse practitioners,
podiatrists, technicians, and receptionists, clerks, or secretaries.
Ambulatory Hospital-Based Events
Ambulatory hospital-based events include visits
to physician and nonphysician providers as well as providers of
unknown type in hospital outpatient departments and emergency
rooms. Same-day hospital discharges (hospital events classified
as inpatient that did not result in an overnight stay) also are
treated as ambulatory hospital-based events in these estimates.
Telephone contact with hospital-based providers is not included
in these estimates.
Hospital Inpatient Events
Hospital stays include all nights spent in
a hospital during calendar year 1996. Population estimates for
total stays have been adjusted for small levels of item nonresponse
for the control variables of perceived health status, usual source
of care, and health insurance status. The number of hospital inpatient
stays in Table 3 is underestimated because some inpatient stays
for newborns were not reported in the MEPS HC. Analysts could
reconstruct inpatient stay estimates by analyzing the 1996 MEPS
utilization data under the assumption that all infants whose mothers
had hospital discharges were delivered in and discharged from
the hospital. Dental Events
In each round of interviews, respondents
were asked to enumerate all dental visits for each family
member. Dental events include visits to general dentists,
dental hygienists, dental technicians, orthodontists, endodontists,
and periodontists.
Home Health Care Events
In each round of interviews, respondents
were asked to provide a monthly summary of home health care
visits for each family member provided by a home health agency,
hospital, nursing home, or self-employed provider, as well
as home health care provided from unpaid informal providers
such as friends, neighbors, or relatives. Estimates in this
report exclude unpaid informal care provided by friends, neighbors,
or family members.
Prescription Medicines
During each interview,
respondents were asked whether or not each family member purchased
or received
any prescription medicine.
Age
The respondent
was asked to report the age of each family member as of
the date of each interview for
Rounds 1, 2, and 3. Unless otherwise specified, in this report
age is based on the sample person’s age as of December
31, 1996. If data were not collected during Round 3 because
the sample person was out of scope (e.g., deceased or institutionalized),
then age at the time of the Round 2 interview was used. Similarly,
if age at Round 2 was not collected because the person was
out of scope, then age at Round 1 was used.
Race/Ethnicity
Classification
by race and ethnicity is based on information reported for each
family member. Respondents were
asked if the race of the sample person was best described as American
Indian, Alaska Native, Asian or Pacific Islander, black, white,
or other. They also were asked if the sample person’s main
national origin or ancestry was Puerto Rican; Cuban; Mexican,
Mexicano, Mexican American, or Chicano; other Latin American;
or other Spanish. All persons whose main national origin or ancestry
was reported in one of these Hispanic groups, regardless of racial
background, are classified as Hispanic. Since the Hispanic grouping
can include black Hispanic, white Hispanic, and other Hispanic,
the race categories of black and white/other do not include Hispanic
persons.
Place of Residence
Individuals are
identified as residing either inside or outside a metropolitan
statistical area (MSA) as designated
by the U.S. Office of Management and Budget (OMB), which applied
1990 standards using population counts from the 1990 U.S. Census.
An MSA is a large population nucleus combined with adjacent communities
that have a high degree of economic and social integration with
the nucleus. Each MSA has one or more central counties containing
the area’s main population concentration. In New England,
metropolitan areas consist of cities and towns rather than whole
counties. MSA data are based on MSA status as of December 31,
1996. If MSA status was not collected during Round 3 because the
sample person was out of scope, then MSA status at Round 1 was
used. Perceived Health Status
Perceived health
status is derived from cross-sectional data collected during Round
1 and represents the sample person’s
status during approximately the first half of 1996. This is the
most current MEPS information available for perceived health status.
The respondent was asked to rate the health of each person in
the family at the time of the Round 1 interview according to the
following categories: excellent, very good, good, fair, and poor.
For Tables 1, 3, and 4, perceived health
status estimates exclude 59 persons because of item nonresponse
in Round 1. Estimates are based on 21,271 persons with positive
full-year weights, representing a weighted population of 264,714,000.
For Table 2, perceived health status estimates
exclude 12 children because of item nonresponse in Round 1.
Estimates are based on 6,016 children with positive full-year
weights, resulting in a weighted population of 68,509,000.
Health Insurance Status
Health insurance status is also derived
from Round 1 data, the most current MEPS data for health insurance
status available. The household respondent was asked if, between
January 1, 1996, and the time of the Round 1 interview, anyone
in the family was covered by any of the sources of public
and private health insurance coverage discussed in the following
paragraphs. For this report, Medicare and CHAMPUS/CHAMPVA
coverage represent coverage as of the date of the Round 1
interview. (CHAMPUS and CHAMPVA are the Civilian Health and
Medical Programs for the Uniformed Services and Veterans Affairs.)
All other sources of insurance represent coverage at any time
during the Round 1 reference period. Persons counted as uninsured
were uninsured throughout the Round 1 reference period. For
additional details on health insurance status measures in
MEPS, see Vistnes and Monheit (1997).
For Tables 1, 3, and 4, health insurance
status estimates exclude 58 persons because of item nonresponse
in Round 1. Estimates are based on 21,271 persons with positive
full-year weights, resulting in a weighted population of 264,714,000.
For Table 2, health insurance status estimates
exclude two children because of item nonresponse in Round
1. Estimates are based on 6,016 children with positive full-year
weights, resulting in a weighted population of 68,476,000.
Public Coverage
For this report, individuals are considered
to have public coverage only if they met both of the following
criteria:
- They were not covered by private insurance.
- They were covered by one of the following
public programs: Medicare, Medicaid, or other public hospital/physician
coverage.
Private Health Insurance
Private health insurance is defined for
this report as insurance that provides coverage for hospital
and physician care. Insurance that provides coverage for a
single service only, such as dental or vision coverage, is
not counted. Coverage by CHAMPUS/CHAMPVA is included as private
health insurance.
Uninsured
The uninsured are defined as persons not
covered by Medicare, CHAMPUS/CHAMPVA, Medicaid, other public
hospital/physician programs, or private hospital/physician
insurance throughout the entire Round 1 reference period.
Individuals covered only by noncomprehensive State-specific
programs (e.g., Maryland Kidney Disease Program, Colorado
Child Health Plan) or private single-service plans (e.g.,
coverage for dental or vision care only, coverage for accidents
or specific diseases) are not considered to be insured.
Usual Source of Care
Usual source
of care was collected in a supplementary module on access
to care administered in Round
2. For each family member, the MEPS interviewer ascertained
whether there is a particular doctor’s office, clinic,
health center, or other place that the individual usually
goes when sick or in need of health advice. Usual source of
care was collected in a supplementary module on access to
care administered in Round 2. For each family member, the
MEPS interviewer ascertains whether there is a particular
doctor’s office, clinic, health center, or other place
that the individual usually goes when sick or in need of health
advice.
For Tables 1, 3, and 4, usual source of
care estimates exclude 156 persons because of missing data
in Round 2. Estimates are based on 21,386 persons with positive
full-year weights, resulting in a weighted population of 265,966,000.
For Table 2, usual
source of care estimates exclude 18 children because of missing
data in Round 2. Estimates
are based on 6,190 children with positive full-year weights,
resulting in a weighted population of 70,413,000.
Table 2 contains two variables that pertain
to the characteristics of parents of children under age 18:
the number of parents living in the home and the highest education
of either parent for children living with at least one parent.
Number of Parents Living in the Home
Number of parents living in the home was
derived from data collected during Round 1. It indicates the
number of parents living in the home at the time of the Round
1 interview and does not account for changes in family structure
that may have occurred during the time period between the
Round 1 interview and December 31, 1996. Estimates are based
on children who were under age 18 as of December 31, 1996.
This resulted in a weighted population of 68,476,000 upon
which estimates are based.
Highest Education of Either Parent
Highest education
of either parent for children living with at least one parent
(181 children were not living
with either parent) was also derived from education data collected
during Round 1. It represents parents’ educational status
at the time of the Round 1 interview.
The sample selected for the 1996 MEPS, a
subsample of the 1995 NHIS, was designed to produce national
estimates that are representative of the civilian noninstitutionalized
population of the United States. Round 1 data were obtained
for approximately 9,400 households in MEPS, resulting in a
survey response rate of 78 percent. This figure reflects participation
in both NHIS and MEPS. For Round 2, the response rate was
95 percent, resulting in a response rate of 74 percent overall
from the NHIS interview through Round 2 of MEPS. For Round
3, the response rate was 95 percent, resulting in a full-year
response rate of 70 percent.
The statistics presented in this report
are affected by both sampling error and sources of nonsampling
error, which include nonresponse bias, respondent reporting
errors, and interviewer effects. For a detailed description
of the MEPS survey design, the adopted sample design, and
methods used to minimize sources of nonsampling error, see
J. Cohen (1997), S. Cohen (1997), and Cohen, Monheit, Beauregard,
et al. (1996).
The MEPS person-level
estimation weights include nonresponse adjustments and poststratification
adjustments
to population totals obtained from the March 1997 Current
Population Survey (CPS) to reflect the Census Bureau estimated
population distribution across age and sex categories as of
December 1996. The person-level poststratification incorporated
the following variables: region, MSA, age, race/ethnicity,
and sex. Overall, the weighted population estimate for the
civilian noninstitutionalized population as of December 31,
1996, is 265,439,511. The inclusion of persons who were in
scope at some time in 1996 but were out of scope (deceased,
institutionalized,active-duty military, or out of the country)
as of December 31, 1996, brings the estimated total number
of persons represented by MEPS respondents over the course
of the year up to 268,130,477.
Tests of statistical
significance were used to determine whether the differences
between populations exist
at specified levels of confidence or whether they occurred
by chance. Differences were tested using Z-scores having asymptotic
normal properties at the 0.05 level of significance. Unless
otherwise noted, only statistically significant differences
between estimates are discussed in the text.
Estimates presented in the tables were
rounded to the nearest 0.1 percent. Standard errors were rounded
to the nearest 0.01. Some of the estimates for population totals
of subgroups presented in the tables will not add exactly to
the overall estimated population total as aconsequence of rounding.
Standard
Error Tables
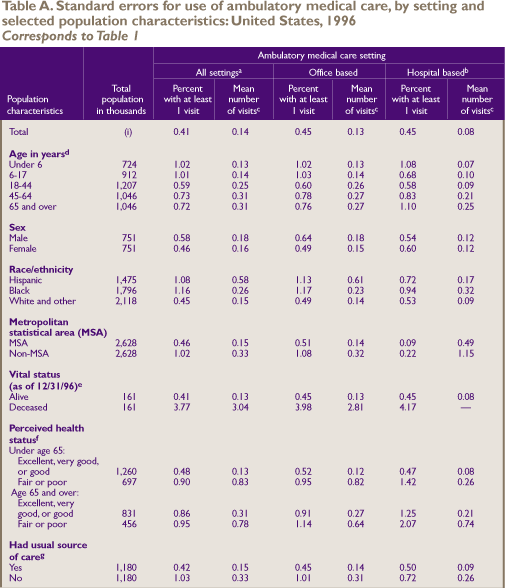
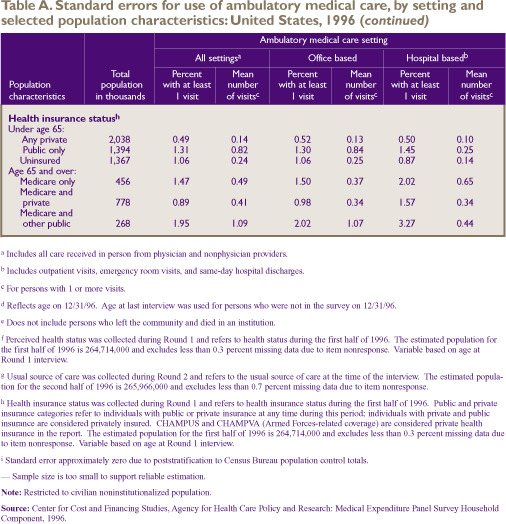
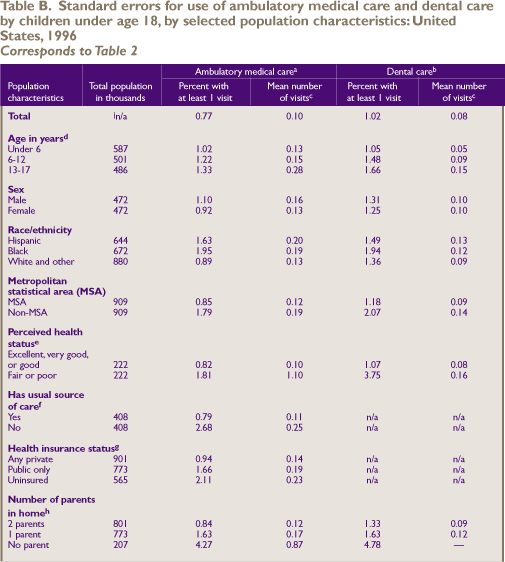
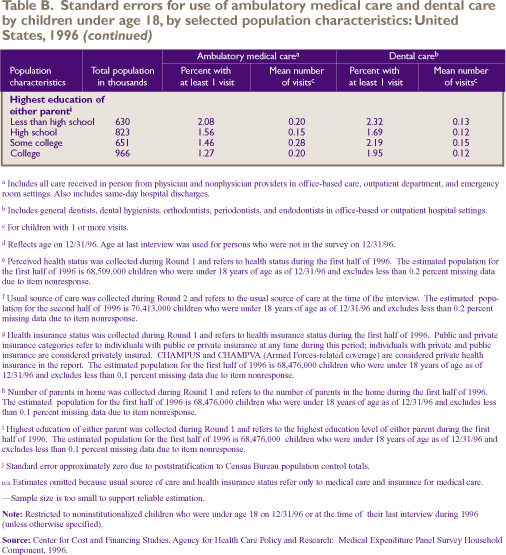
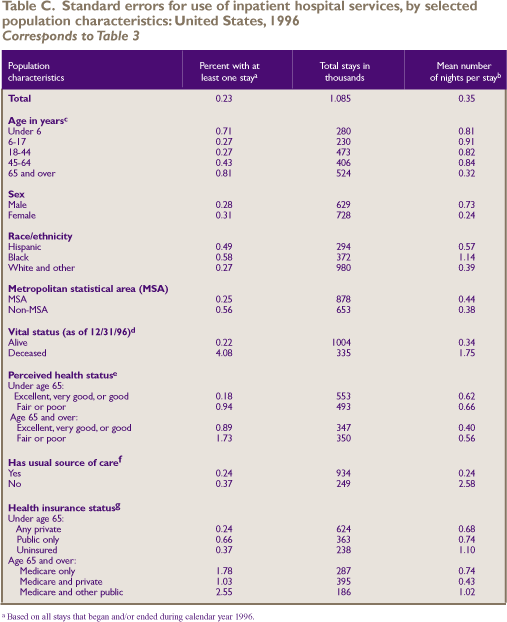

^top
Suggested
Citation: Research Findings #7: Use of Health Care Services, 1996. March 1999. Agency
for Healthcare Research and Quality, Rockville,
MD. http://www.meps.ahrq.gov/data_files/publications/rf7/rf7.shtml
|
|
