
|
|
Font Size:
|
||||
|
|
|
|
||||
STATISTICAL BRIEF #454:
Expenditures for Mental Health among Adults, Ages 18-64, 2009-2011: Estimates for the U.S. Civilian Noninstitutionalized Population
Highlights
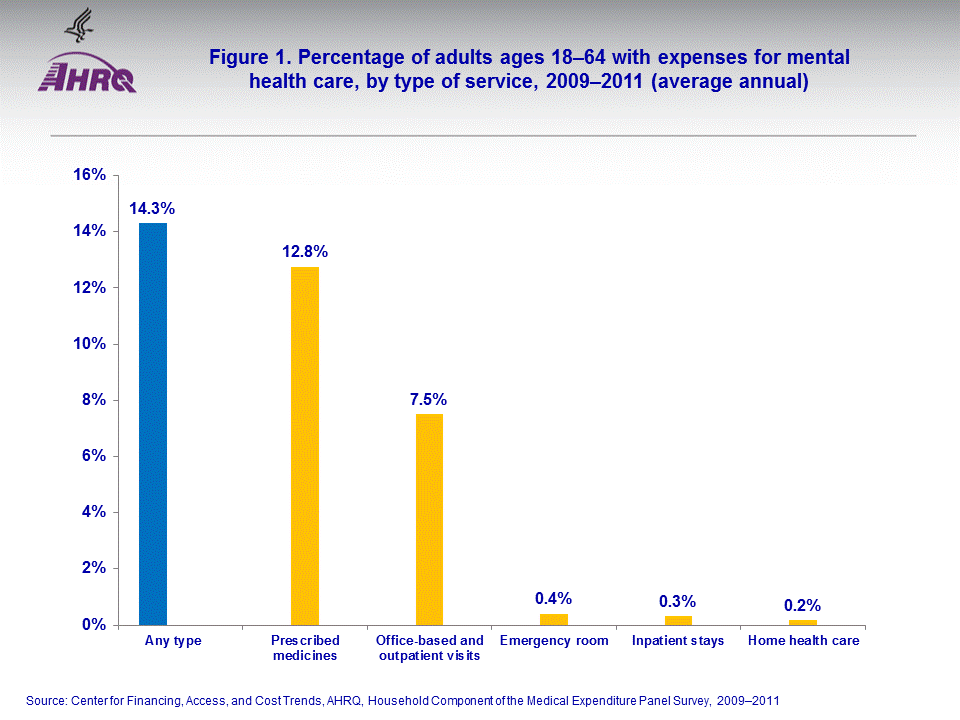
- An annual average of 27.5 million adults ages 18-64 (14.3 percent of adults in that age range) had some health care expenses for mental health disorders in 2009-2011.
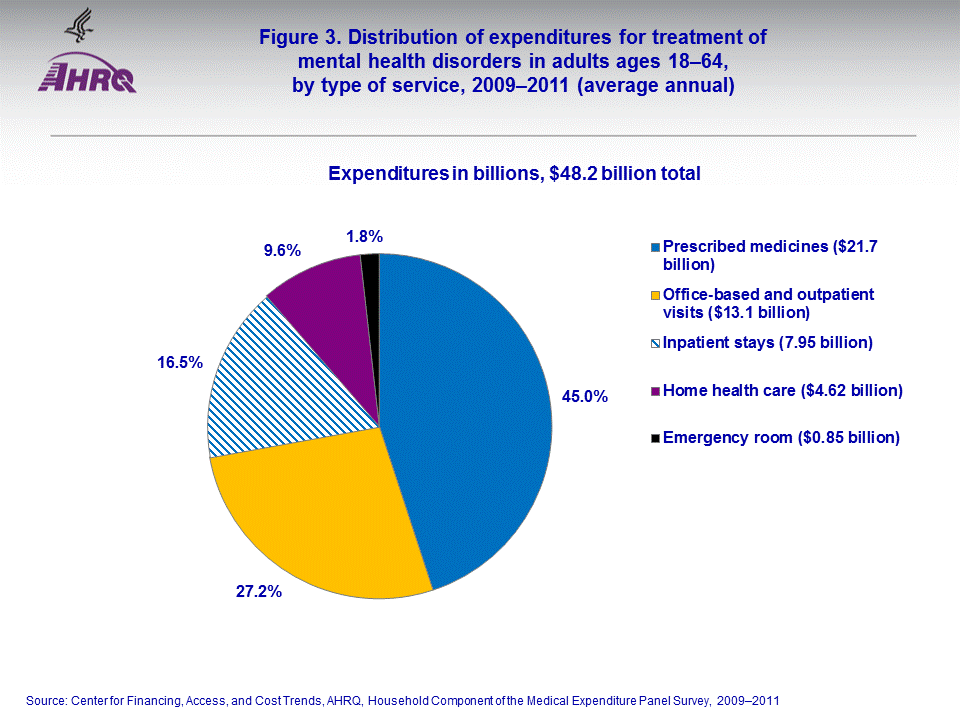
- Average annual direct spending to treat mental health disorders in adults ages 18-64 totaled $48.2 billion (in 2011 dollars) during 2009-2011, with 45.0 percent ($21.7 billion) going towards prescription medicines.
- Average annual mental health-related expenditures for adults ages 18-64 with mental health-related expenditures in 2009-2011 were $1,751 per person in 2011 dollars.
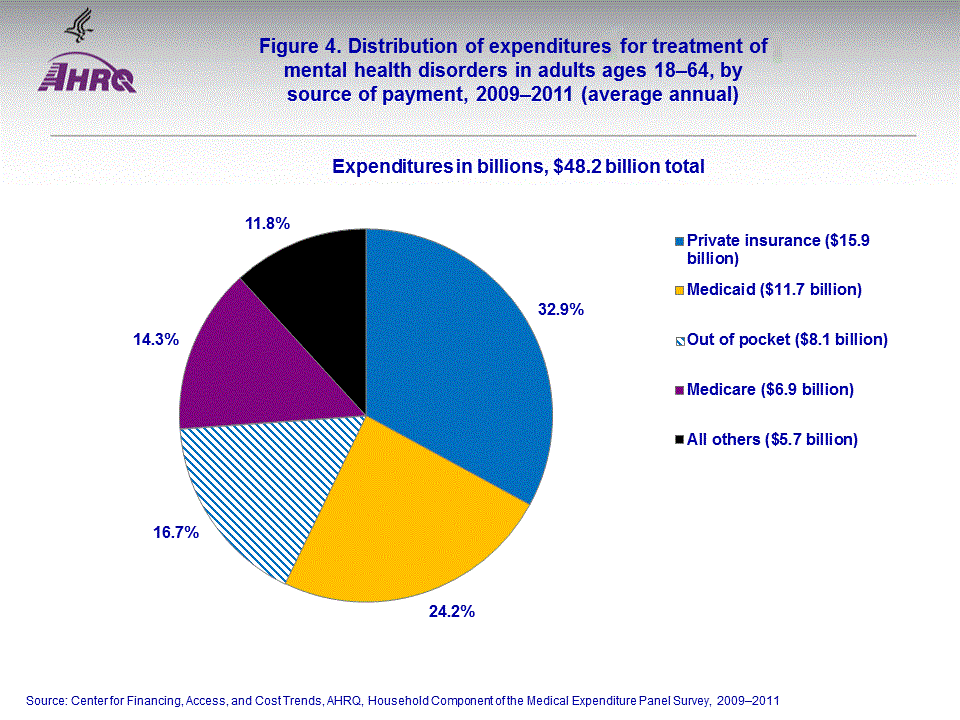
- About one-third of expenditures for treatment of mental health disorders for adults ages 18-64 were paid for by private insurance. Medicaid covered 24.2 percent, out-of-pocket expenses constituted 16.7 percent of expenses, and Medicare paid for 14.3 percent. The remaining expenditures were covered by sources such as veterans' benefits, TRICARE, Workers' Compensation, governmental aid, and other sources of private and public insurance.
Introduction
This Statistical Brief presents estimates based on the Household Component of the Medical Expenditure Panel Survey (MEPS-HC) on the use of and expenditures related to mental health disorders among adults ages 18 to 64 in the U.S. civilian noninstitutionalized population. Average annual estimates for 2009–2011 are shown by source of payment. Expenditures for pooled years are expressed in constant dollars by inflating those for 2009–10 to 2011 U.S. dollars using the Personal Health Care Expenditure (PHCE) price index component of the National Health Expenditure Accounts (http://www.meps.ahrq.gov/mepsweb/about_meps/Price_Index.shtml). Except where noted, all differences between estimates noted in the text are statistically significant at the 0.05 level or better.Findings
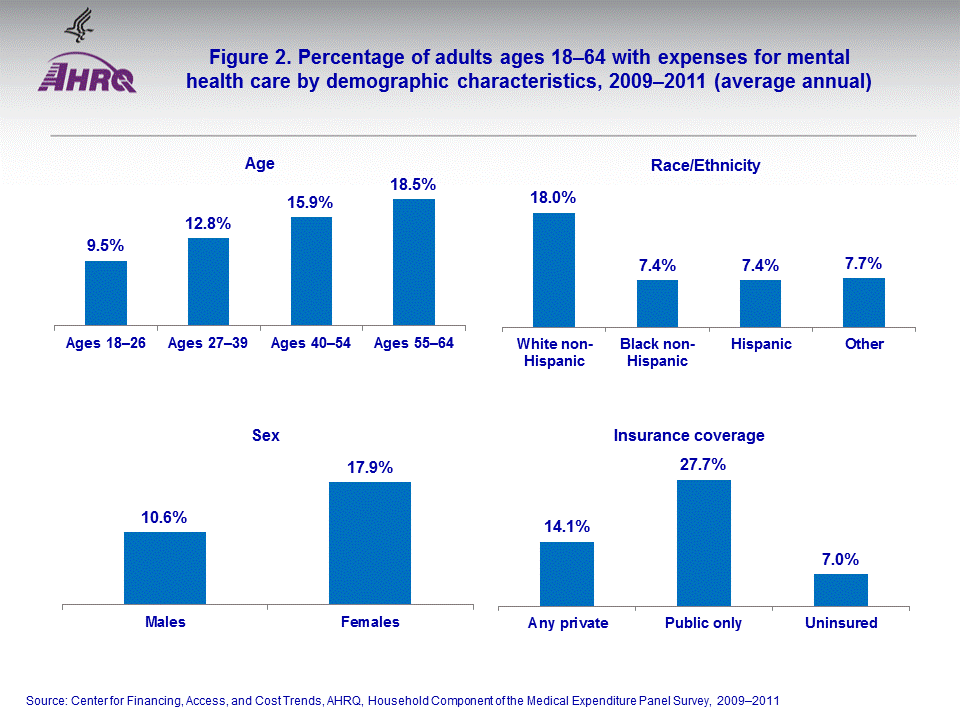
An annual average of 14.3 percent (figure 1) of adults ages 18–64 (about 27.5 million adults) had expenses for treatment for mental health disorders in 2009–2011. The majority of these individuals (12.8 percent of adults ages 18–64) received prescription medications for mental health disorders. Of adults ages 18–64, 7.5 percent had an office-based or outpatient medical visit for a mental health disorder, while fewer than 1 percent had an inpatient stay, emergency room visit, or home health visit. Of those adults ages 18–64 in 2009–2011 who had a mental health-related expense, the average annual total expense on mental health was $1,751 (data not shown).Among adults ages 18–64, the likelihood of having mental health-related expenses increased with age (figure 2) from only 9.5 percent of those ages 18–26, to 12.8 percent of those ages 27–39, to 15.9 percent of those ages 40–54, and 18.5 percent of those ages 55–64. Women (17.9 percent) were more likely than men (10.6 percent) to have had an expense for treatment of a mental health disorder. In this age group, non-Hispanic white adults (18.0 percent) were more than twice as likely as non-Hispanic black adults (7.4 percent), Hispanic adults (7.4 percent), or all other adults (7.7 percent) to have had mental health-related expenses (the difference among the latter three groups is not statistically significant). Adults below the poverty level were more likely than non-poor adults (18.6 percent versus 13.6 percent, not shown) to have received mental health treatment, but there were no significant differences among subgroups of non-poor adults (i.e., near-poor, low income, middle income, and high income individuals). Adults who only had public insurance (27.7 percent) were much more likely than adults with any private insurance (14.1 percent) or uninsured adults (7.0 percent) to have had a mental health-related expense.
Nearly one-third (32.9 percent) of expenditures for treatment of mental health disorders for adults ages 18–64 was paid for by private insurance (figure 4). Medicaid covered 24.2 percent, out-of-pocket expenses constituted 16.7 percent of expenses, and Medicare paid for 14.3 percent. The remaining expenditures were covered by sources such as veterans' benefits, TRICARE, Workers' Compensation, governmental aid, and other sources of private and public insurance.
Data Source
The estimates shown in this Statistical Brief are based on data from the following MEPS data files for 2009–2011: Full Year Consolidated (HC-129, HC-138, HC-147); Prescribed Medicines (HC-126A, HC-135A, HC-144A); Hospital Inpatient Stays (HC-126D, HC-135D, HC-144D); Emergency Room Visits (HC-126G, HC-135G, HC-144G); Hospital Outpatient Visits (HC-126G, HC-135G, HC-144G); Office-Based Medical Provider Visits (HC-126G, HC-135G, HC-144G).Definitions
Mental health disordersThis Brief analyzes adults ages 18–64 and their expenditures related to mental health disorders. The conditions reported by respondents were recorded by interviewers as verbatim text which were then coded by professional coders to fully specified ICD-9-CM codes. These codes were regrouped in clinically homogenous categories known as CCS codes. Conditions with CCS codes 650–670 (mental health) were used for this Brief. A crosswalk of ICD-9 codes and CCS codes is available in the documentation file of the Medical Conditions File. For additional information on crosswalk between ICD-9 codes and CCS codes, please visit: http://www.hcup-us.ahrq.gov/toolssoftware/ccs/ccs.jsp.
Expenditures
Expenditures associated with treated medical conditions in MEPS are defined as payments from all sources for hospital inpatient care, ambulatory care provided in offices and hospital outpatient departments, care provided in emergency departments, paid care provided in the patient's home (home health), and the purchase of prescribed medications. Sources include direct payments from individuals, private insurance, Medicare, Medicaid, Workers' Compensation, and miscellaneous other sources. Payments for over-the-counter drugs are not included in MEPS total expenditures. Indirect payments not related to specific medical events, such as Medicaid Disproportionate Share and Medicare Direct Medical Education subsidies, are also excluded.
Expenditures were classified as being associated with mental health if a visit, stay, or medication purchase was cited as being related to mental health. Expenditures may be associated with more than one condition and therefore may include some spending for conditions other than mental health. Total spending does not include amounts paid for other medical expenses, such as durable and nondurable supplies, medical equipment, eyeglasses, ambulance services, and dental expenses, because these items are not linked to specific conditions in MEPS.
Health insurance status
Individuals were classified in the following three insurance categories based on household responses to health insurance status questions:
- Any private health insurance: Individuals who, at any time during the year, had insurance that provides coverage for hospital and physician care (other than Medicare, Medicaid, or other public hospital/physician coverage) were classified as having private insurance. Coverage by TRICARE (Armed Forces-related coverage) was also included as private health insurance. Insurance that provides coverage for a single service only, such as dental or vision coverage, was not included.
- Public coverage only: Individuals were considered to have public coverage only if they met both of the following criteria: 1) they were not covered by private insurance at any time during the year; and 2) they were covered by any of the following public programs at any point during the year: Medicare, Medicaid, or other public hospital/physician coverage.
- Uninsured: The uninsured were defined as people not covered by private hospital/physician insurance, Medicare, TRICARE, Medicaid, or other public hospital/physician programs at any time during the entire year or period of eligibility for the survey.
- Private insurance: This category includes payments made by insurance plans covering hospital and other medical care (excluding payments from Medicare, Medicaid, and other public sources), Medigap plans, and TRICARE (Armed Forces-related coverage).
- Medicare: Medicare is a federally financed health insurance plan for the elderly, persons receiving Social Security disability payments, and persons with end-stage renal disease. Medicare Part A, which provides hospital insurance, is automatically given to those who are eligible for Social Security. Medicare Part B provides supplementary medical insurance that pays for medical expenses and can be purchased for a monthly premium. Medicare Part D, which started in 2006, covers prescription drug expenses.
- Medicaid/CHIP: This category includes payments made by the Medicaid and CHIP programs which are means-tested government programs financed jointly by federal and state funds that provide health care to those who are eligible. Medicaid is designed to provide health coverage to families and individuals who are unable to afford necessary medical care while CHIP provides coverage to additional low income children not eligible for Medicaid. Eligibility criteria for both programs vary significantly by state.
- Out of pocket: This category includes expenses paid by the user or other family member.
- Other sources: This category includes payments from other federal sources such as Indian Health Service, military treatment facilities, and other care provided by the federal government; various state and local sources (community and neighborhood clinics, state and local health departments, and state programs other than Medicaid/CHIP); various unclassified sources (e.g., automobile, homeowner's, or other liability insurance, and other miscellaneous or unknown sources); Medicaid/CHIP payments reported for persons who were not reported as enrolled in the Medicaid or CHIP programs at any time during the year; and private insurance payments reported for persons without any reported private health insurance coverage during the year.
About MEPS-HC
MEPS-HC is a nationally representative longitudinal survey that collects detailed information on health care utilization and expenditures, health insurance, and health status, as well as a wide variety of social, demographic, and economic characteristics for the U.S. civilian noninstitutionalized population. It is cosponsored by the Agency for Healthcare Research and Quality and the National Center for Health Statistics.For more information about MEPS, call the MEPS information coordinator at AHRQ (301-427-1406) or visit the MEPS Web site at http://www.meps.ahrq.gov/.
References
For a detailed description of the MEPS survey design, sample design, and methods used to minimize sources of nonsampling errors, see the following publications:Cohen, J. Design and Methods of the Medical Expenditure Panel Survey Household Component. MEPS Methodology Report No. 1. AHCPR Pub. No. 97-0026. Rockville, MD. Agency for Health Care Policy and Research, 1997. http://www.meps.ahrq.gov/mepsweb/data_files/publications/mr1/mr1.shtml
Cohen, S. Sample Design of the 1996 Medical Expenditure Panel Survey Household Component. MEPS Methodology Report No. 2. AHCPR Pub. No. 97-0027. Rockville, MD. Agency for Health Care Policy and Research, 1997. http://www.meps.ahrq.gov/mepsweb/data_files/publications/mr2/mr2.shtml
Cohen, S. Design Strategies and Innovations in the Medical Expenditure Panel Survey. Medical Care, July 2003: 41(7) Supplement: III-5–III-12.
Ezzati-Rice, T.M., Rohde, F., Greenblatt, J. Sample Design of the Medical Expenditure Panel Survey Household Component, 1998–2007. Methodology Report No. 22. March 2008. Agency for Healthcare Research and Quality, Rockville, MD. http://www.meps.ahrq.gov/mepsweb/data_files/publications/mr22/mr22.shtml
For more information about mental health disorders, see the following:
Mental Health Fact Sheet: http://www.cdc.gov/nchs/fastats/mental-health.htm
Suggested Citation
Zibman, C. Expenditures for Mental Health among Adults, Ages 18–64, 2009–2011: Estimates for the U.S. Civilian Noninstitutionalized Population. Statistical Brief #454. October 2014. Agency for Healthcare Research and Quality, Rockville, MD. http://www.meps.ahrq.gov/mepsweb/data_files/publications/st454/stat454.shtmlAHRQ welcomes questions and comments from readers of this publication who are interested in obtaining more information about access, cost, use, financing, and quality of health care in the United States. We also invite you to tell us how you are using this Statistical Brief and other MEPS data and tools and to share suggestions on how MEPS products might be enhanced to further meet your needs. Please email us at MEPSProjectDirector@ahrq.hhs.gov or send a letter to the address below:
Steven B. Cohen, PhD, Director
Center for Financing, Access, and Cost Trends
Agency for Healthcare Research and Quality
540 Gaither Road
Rockville, MD 20850
 |
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||
 |
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||
 |
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||
 |
||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||


