
|
|
Font Size:
|
||||
|
|
|
|
||||
STATISTICAL BRIEF #185:
Co-pays, Deductibles, and Coinsurance for Employer-Sponsored Health Insurance in the State and Local Government Workforce, by Census Division, 2005
Highlights
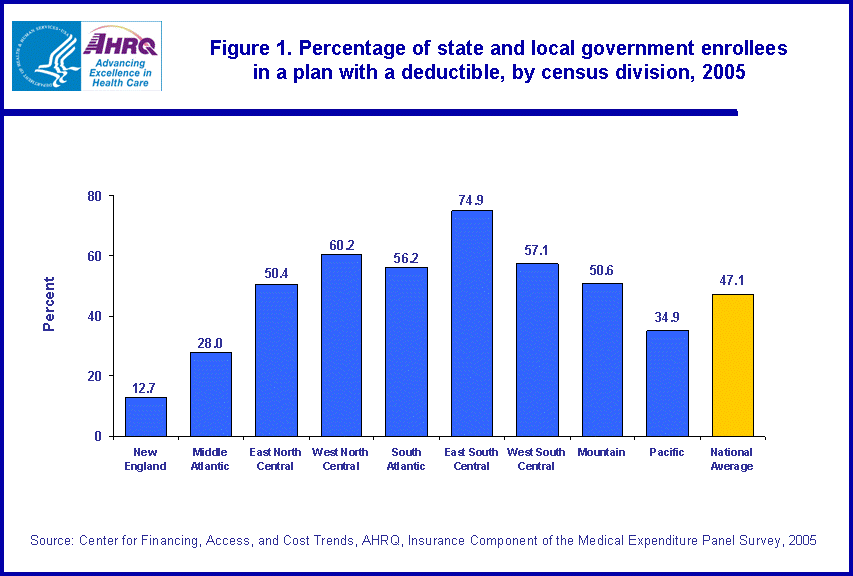
- In 2005, 47.1 percent of state and local government employees enrolled in employer-sponsored health insurance were required to pay a deductible by their health insurance plan.
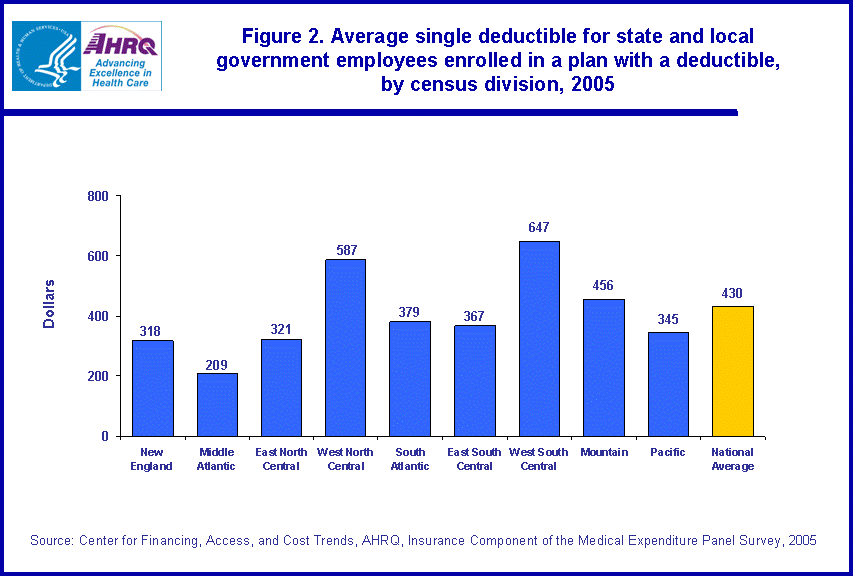
- In 2005, state and local government employees enrolled in employer-sponsored health insurance who were responsible for a deductible had an average single deductible of $430 and an average family deductible of $885. Both of these values varied significantly by an employee's census division.
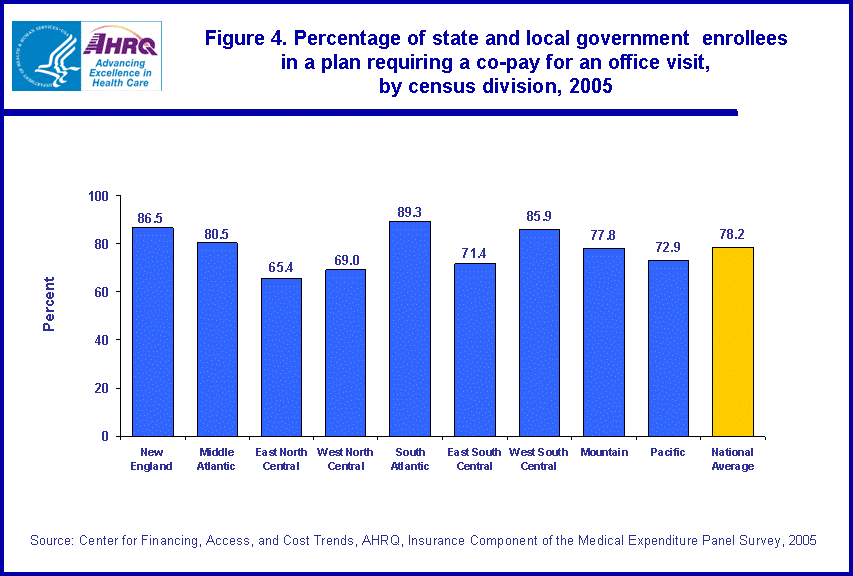
- In 2005, 78.2 percent of state and local government employees enrolled in employer-sponsored health insurance paid a co-pay for each doctor visit. The average dollar co-pay among these enrollees was $15.59. These values varied significantly by census division.
- The average coinsurance percentage for a doctor visit for employees from state and local governments enrolled in employer-sponsored health insurance with a coinsurance was 17.7 percent in 2005.
Introduction
Employer-sponsored health insurance is the primary source of health insurance coverage in the United States for active employees. It is especially important to the 19.05 million state and local government employees. According to data from the Insurance Component of the 2005 Medical Expenditure Panel Survey (MEPS-IC), 99.9% of state and local government employees work where health insurance is offered and 66.8 percent of these employees are enrolled in employer-sponsored health insurance. Both these figures are significantly higher than the same values for private sector employees.
In recent years, premiums and employee contributions for employer-sponsored health insurance provided by state and local governments have risen dramatically. For instance, annual employee contributions towards family coverage for state and local government employees rose from $1,267 to $2,058 (62.4 percent) between 2000 and 2005. Contribution costs are only a portion of the costs of health insurance for these employees. Other factors, such as whether an employee has a deductible, the size of deductibles, and the size of co-pays and coinsurance, also contribute to employees' out-of-pocket cost of care.
This Statistical Brief examines the levels of these deductibles, co-pays, and coinsurance for state and local government employees and how they vary by census division. Among the items examined are the percentage of enrollees who paid a deductible and the size of deductibles, what percentage of enrollees paid co-pays and the size of co-pays, and the average coinsurance percentage paid by enrollees. Only estimates that had a statistically significant difference from the national average at the 0.05 percent significance level are noted in the text.
Findings
Among the 12.7 million state and local government employees enrolled in employer-sponsored health insurance in 2005, 47.1 percent were enrolled in a plan that required they meet an annual deductible (figure 1). This percentage varied significantly by census division. A higher than average percentage of enrollees from governments in the West North Central, South Atlantic, East South Central and West South Central census divisions, 60.2, 56.2, 74.9, and 57.1 percent, respectively, had plans with a deductible. A lower than average percentage of the enrollees in the New England, Middle Atlantic, and Pacific census divisions had a plan with a deductible. In these census divisions, 12.7, 28.0, and 34.9 percent, respectively, of the enrollees had plans with a deductible in 2005.
Among enrollees from state and local governments who were responsible for a deductible, the size of both single and family deductibles varied by census division in 2005. The average amount of the single deductible for enrolled state and local employees who paid a deductible was $430 (figure 2). Enrollees who were responsible for deductibles in governments in the West North Central and West South Central census divisions had higher than average single deductibles of $587 and $647, respectively. Enrollees from governments in the New England, Middle Atlantic, East North Central, East South Central, and Pacific census divisions who were responsible for a deductible had lower than average single deductibles of $318, $209, $321, $367, and $345, respectively.
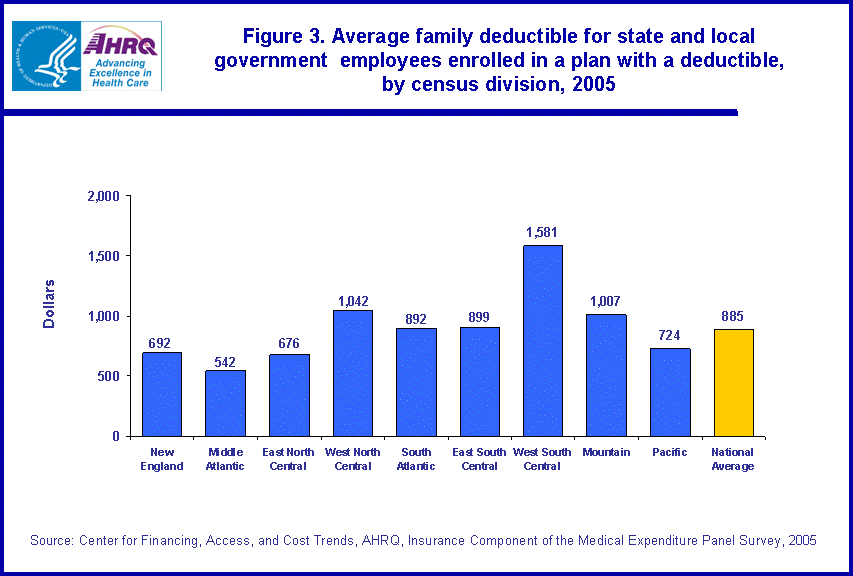
Among those enrollees who had deductibles, those in the West North Central and West South Central census divisions had family deductibles higher than the national state and local government average of $885 (figure 3). These enrollees were responsible for average family deductibles of $1,042 and $1,581, respectively. Enrollees with deductibles in state and local governments in the New England, Middle Atlantic, East North Central, and Pacific census divisions had average family deductibles of $692, $542, $676, and $724, respectively. These values were all significantly less than the national state and local government average.
In 2005, 78.2 percent of state and local government enrollees in employer-sponsored health insurance paid a co-pay for an office visit (figure 4). In the New England, South Atlantic, and West South Central census divisions, the percentages were higher than average, at 86.5, 89.3, and 85.9 percent, respectively. In the East North Central, West North Central, East South Central, and Pacific census divisions, lower than average percentages of enrollees paid a co-pay. In these census divisions, 65.4, 69.0, 71.4, and 72.9 percent, respectively, of enrollees paid a co-pay.
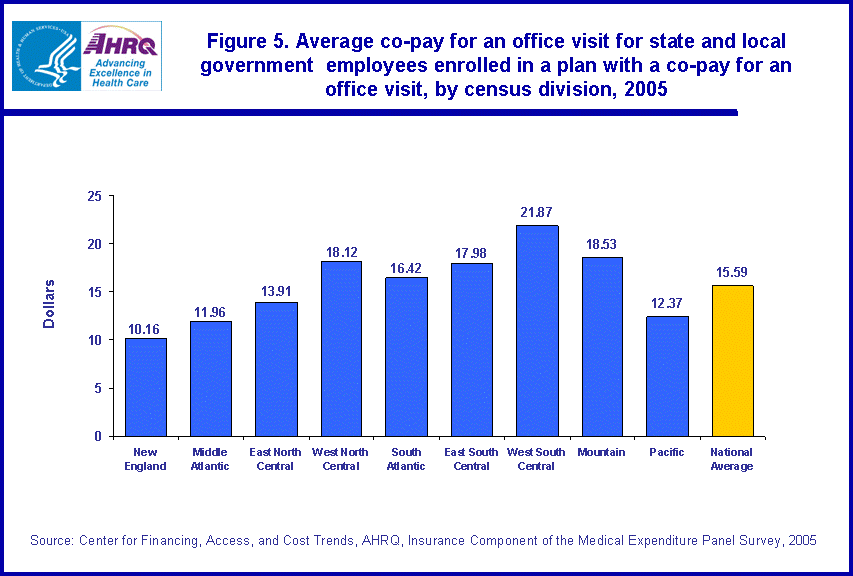
The average co-pay for an office visit for enrollees among state and local government employees in plans with co-pays was $15.59 (figure 5). Enrollees with co-pays in the West North Central, East South Central, West South Central, and Mountain census divisions paid higher than average amounts of $18.12, $17.98, $21.87, and $18.53, respectively. Enrollees from state and local governments in the New England, Middle Atlantic, East North Central, and Pacific census divisions paid lower than average co-pays of $10.16, $11.96, $13.91, and $12.37, respectively.
Persons who do not have co-pays generally have a coinsurance percentage to pay. For state and local government enrollees in 2005, the average coinsurance percentage for an office visit for those enrollees who paid a coinsurance percentage was 17.7 percent (figure 6). Enrollees from governments in the Pacific census division who had a coinsurance, paid a lower than average rate of 14.6 percent, while those from the Middle Atlantic, West North Central, West South Central, and Mountain census divisions paid higher than average coinsurance rates of 19.6, 22.4, 19.5, and 20.3 percent, respectively.
Data Source
This Statistical Brief summarizes data from the 2005 MEPS-IC. The data are available on the MEPS Web site at http://www.meps.ahrq.gov/mepsweb/data_stats/quick_tables.jsp or have been produced using special computation runs on the confidential MEPS-IC data available at the U.S. Census Bureau.
Definitions
Employer
An employer is defined as either a private sector firm or a state or local government. A private sector firm is defined as a business entity that controls one or more business establishments or locations. Consequently, an employer can have multiple work locations.
Deductible
A deductible is a fixed dollar amount during the benefit period, usually a year, that an insured person pays before the insurer starts to make payments for covered medical services. Plans may have both per individual and family deductibles. Some plans may have separate deductibles for specific services. For example, a plan may have a hospitalization deductible per admission. Deductibles may differ if services are received from an approved provider or if received from providers not on the approved list.
Co-pay
A co-pay is a form of medical cost sharing in a health insurance plan that requires an insured person to pay a fixed dollar amount when a medical service is received, regardless of the total charge for service. The insurer is responsible for the rest of the reimbursement. There may be separate co-pays for different services. For example, an enrollee may pay a $10 co-pay for each doctor's office visit, $75 for each day in the hospital, and $5 for each prescription. Some plans require that a deductible first be met for some specific services before a co-pay applies.
Coinsurance
Coinsurance is a form of medical cost sharing in a health insurance plan that requires an insured person to pay a stated percentage of medical expenses after the deductible amount, if any, has been paid. Once any deductible amount and coinsurance are paid, the insurer is responsible for the rest of the reimbursement for covered benefits up to allowed charges; the individual could also be responsible for any charges in excess of what the insurer determines to be "usual, customary, and reasonable." Coinsurance rates may differ if services are received from an approved provider (i.e., a provider with whom the insurer has a contract or an agreement specifying payment levels and other contract requirements) or if received by providers not on the approved list. In addition to overall coinsurance rates, rates may also differ for different types of services.
Census division
States were grouped into nine census divisions as follows:
- New England: Connecticut, Maine, Massachusetts, New Hampshire, Rhode Island, Vermont
- Middle Atlantic: New Jersey, New York, Pennsylvania
- East North Central: Illinois, Indiana, Michigan, Ohio, Wisconsin
- West North Central: Iowa, Kansas, Minnesota, Missouri, Nebraska, North Dakota, South Dakota
- South Atlantic: Delaware, District of Columbia, Florida, Georgia, Maryland, North Carolina, South Carolina, Virginia, West Virginia
- East South Central: Alabama, Kentucky, Mississippi, Tennessee
- West South Central: Arkansas, Louisiana, Oklahoma, Texas
- Mountain: Arizona, Colorado, Idaho, Montana, Nevada, New Mexico, Utah, Wyoming
- Pacific: Alaska, California, Hawaii, Oregon, Washington
About MEPS-IC
The MEPS-IC is a survey of business establishments and governments that collects information on employer-sponsored health insurance, such as whether insurance is offered, enrollments, types of plans, and premiums. The survey is conducted annually by the U. S. Census Bureau under the sponsorship of the Agency for Healthcare Research and Quality (AHRQ). The yearly response rate has averaged 78 percent for in-scope sample units. Approximately 4 percent of the original sample has been out-of-scope in a typical year. A total sample of 42,000 establishments was selected for the 2005 survey, prior to accounting for losses due to nonresponse and out-of-scope cases.
For more information on this survey, see MEPS Methodology Reports 6, 8, 10, 14, 17, and 18 on the MEPS Web site at http://www.meps.ahrq.gov/mepsweb/data_stats/publications.jsp and Insurance Component Survey Basics at http://www.meps.ahrq.gov/mepsweb/survey_comp/Insurance.jsp.
Suggested Citation
Sommers, J. P. Co-pays, Deductibles, and Coinsurance Percentages for Employer-Sponsored Health Insurance in the State and Local Government Workforce, by Census Division, 2007. Statistical Brief #185. September 2007. Agency for Healthcare Research and Quality, Rockville, Md. http://www.meps.ahrq.gov/mepsweb/data_files/publications/st185/stat185.shtml
AHRQ welcomes questions and comments from readers of this publication who are interested in obtaining more information about access, cost, use, financing, and quality of health care in the United States. We also invite you to tell us how you are using this Statistical Brief and other MEPS data and tools and to share suggestions on how MEPS products might be enhanced to further meet your needs. Please e-mail us at mepsprojectdirector@ahrq.hhs.gov or send a letter to the address below:
Steven B. Cohen, PhD, Director
Center for Financing, Access, and Cost Trends
Agency for Healthcare Research and Quality
540 Gaither Road
Rockville, MD 20850
 |
||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||||||||||
 |
||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||||||||||
 |
||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||||||||||
 |
||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||||||||||
 |
||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||||||||||
 |
||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||||||||||


