
|
|
Font Size:
|
||||
|
|
|
|
||||
STATISTICAL BRIEF #460:
Enrollment in High Premium Employer-Sponsored Health Insurance by State: Private Industry, 2013
Highlights
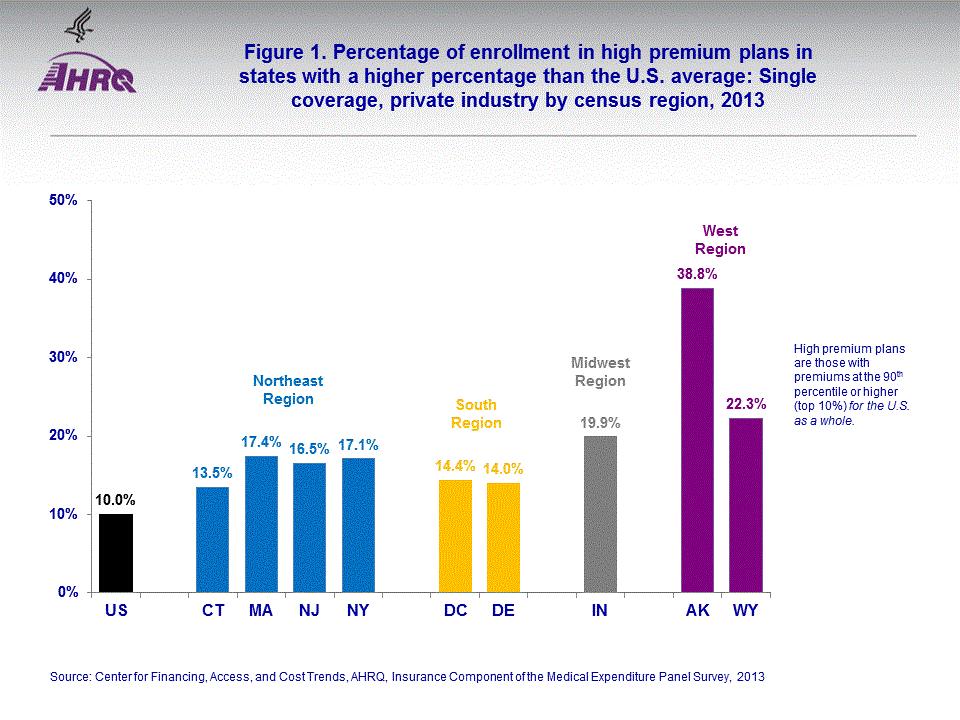
- Nine states, including the District of Columbia, had a larger percentage of enrollees in single coverage employer-sponsored health insurance with a high premium ($7,800 or more, dollar amounts not shown) than the national average of 10 percent in 2013.
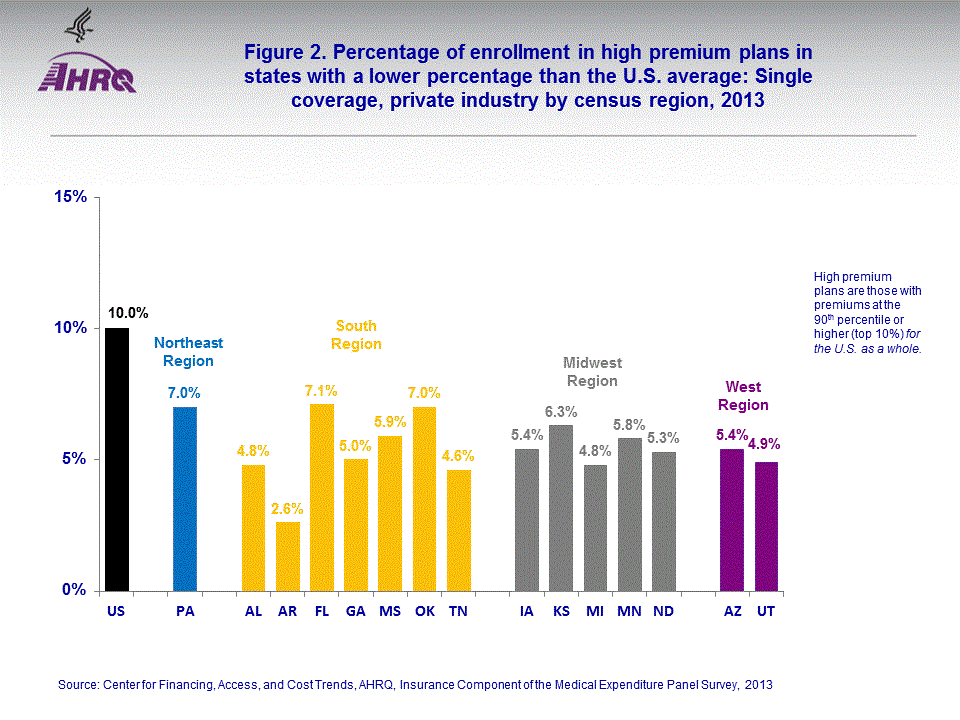
- There were 15 states with a smaller percentage of enrollees in single coverage employer-sponsored health insurance in high premium plans than in the U.S. as a whole; seven of these states were in the South Region and five were in the Midwest Region.
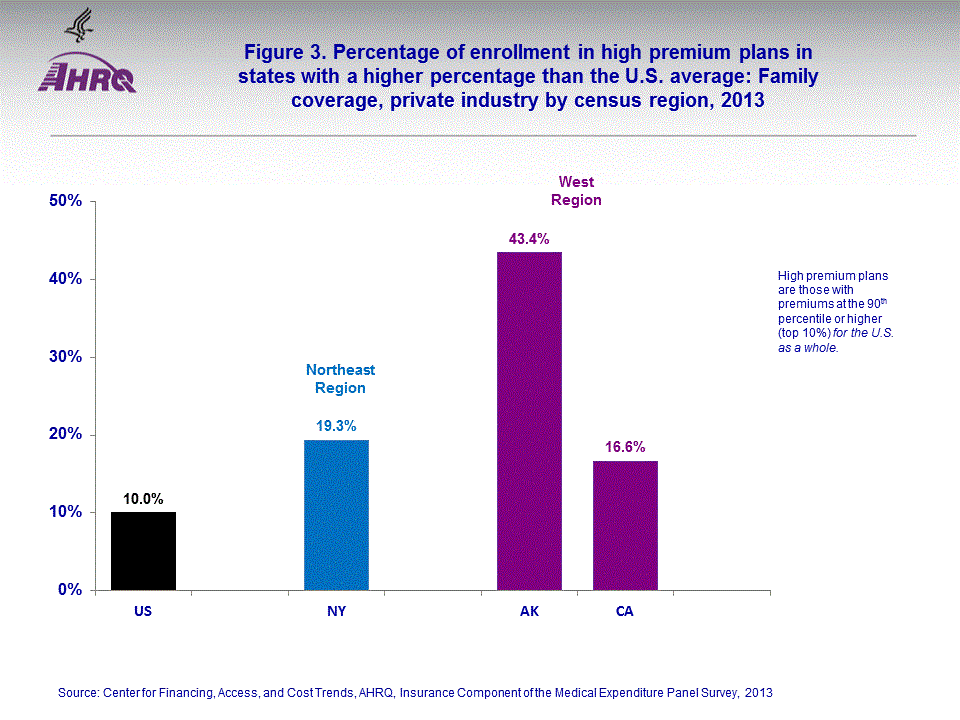
- Only three states had a larger percentage of enrollees in employer-sponsored family coverage with a high premium ($22,000) than the national average of 10 percent—New York in the Northeast Region and Alaska and California in the West Region.
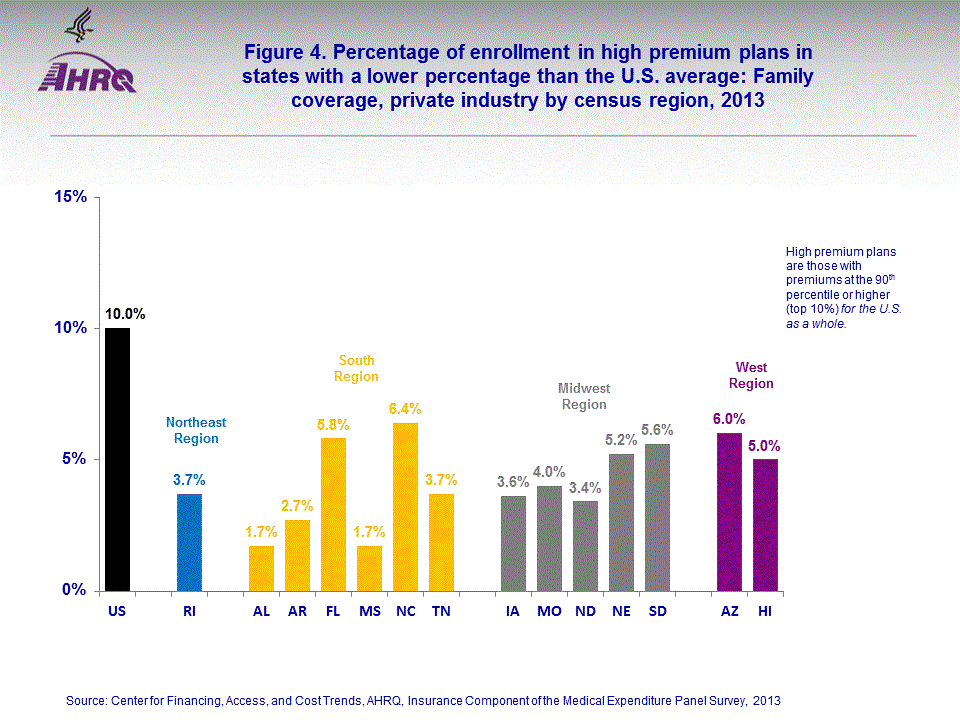
- In 2013, 14 states had a smaller percentage of enrollees with high premium plans in employer-sponsored family coverage than the 10 percent national average. Most of these states were in the South or Midwest Region.
Introduction
This Statistical Brief reports estimates by state on the percentage of private sector employees enrolled in employer-sponsored health insurance plans with high premiums, which are defined as those annual premiums greater than or equal to the 90 percentile for single coverage plans ($7,800), and greater than or equal to the 90 percentile for family coverage plans ($22,000). That is, of all enrollees across the U.S. within each coverage type, 10 percent had premiums at or above these amounts. These estimates were obtained using data from the 2013 Medical Expenditure Panel Survey Insurance Component (MEPS-IC).Estimates are reported by state grouped by census region (Northeast, Midwest, South, and West) and are the percentages of enrollees in single and family coverage that have premiums at the 90th percentile amount or higher. It should be noted that factors other than location can affect premiums. Other factors include benefit packages that are more or less generous (through the absence or presence of deductibles and co-pays, for example), employer characteristics (such as firm size and industry), and demographic factors (such as age and health of enrollees).
All estimates discussed in the text are significantly different from the overall 90th percentile estimates of the U.S. at the 0.05 level unless otherwise noted.
Findings
Figure 1 shows all states that had a larger percentage of enrollees with a high premium (greater than or equal to $7,800) than the U.S. average of 10 percent for private-sector employer-sponsored single coverage in 2013. The percentages ranged from 38.8 percent for Alaska to 13.5 percent for Connecticut. Of the nine states with a larger percentage of enrollees in single coverage plans with premiums greater than or equal to the 90 percentile for the U.S., four were located in the Northeast Region of the United States. In addition to Connecticut, other Northeast states included Massachusetts (17.4 percent), New Jersey (16.5 percent), and New York (17.1 percent). Of the remaining five states with a larger percentage of enrollees in single coverage plans with premiums greater the 10th percentile for the U.S., two were located in the South Region (Delaware, 14.0 percent and the District of Columbia, 14.4 percent), one was in the Midwest Region (Indiana, 19.9 percent), and one state in addition to Alaska was located in the West Region (Wyoming, 22.3 percent).In figure 2, those states shown had a smaller percentage than the U.S. average of 10 percent of enrollees in employer-sponsored single coverage plans with premiums greater than or equal to $7,800 in 2013. The percentages ranged from 7.1 percent for Florida to 2.6 percent for Arkansas in 2013. Of the 15 states listed, one was in the Northeast Region (Pennsylvania, 7.0 percent). In addition to Florida and Arkansas, five additional states were in the South Region (Alabama, 4.8 percent; Georgia, 5.0 percent; Mississippi, 5.9 percent; Oklahoma, 7.0 percent; and Tennessee, 4.6 percent). Five states were located in the Midwest Region (Iowa, 5.4 percent; Kansas, 6.3 percent; Michigan, 4.8 percent; Minnesota, 5.8 percent; and North Dakota, 5.3 percent). Two states were located in the West Region (Arizona, 5.4 percent and Utah, 4.9 percent).
The 14 states with smaller percentages than the U.S. average of 10 percent for private sector enrollees in high premium ($22,000 or higher) family health coverage are shown in figure 4. The percentages ranged from 1.7 percent for both Alabama and Mississippi to 6.4 percent in North Carolina. Only one Northeast Region state was found to have a smaller percentage of enrollees in high premium employer-sponsored family health coverage than the U.S. average (Rhode Island, 3.7 percent). In addition to Alabama, Mississippi, and North Carolina, three states located in the South Region had a smaller percentage of family plan enrollees than the U.S. average (Arkansas, 2.7 percent; Florida, 5.8 percent; and Tennessee, 3.7 percent). The Midwest Region had five states with a smaller percentage of enrollees than the U.S. average with high premiums of 10 percent (Iowa, 3.6 percent; Missouri, 4.0 percent; North Dakota, 3.4 percent; Nebraska, 5.2 percent; and South Dakota, 5.6 percent). Two West Region states had a smaller percentage of enrollees covered by high-premium employer sponsored plans than the U.S. average (Arizona, 6.0 percent and Hawaii, 5.0 percent).
Only New York and Alaska had a larger percentage of private sector enrollees in high premium coverage (greater than the 10 percent U.S. average) for both single and family plans in 2013. Several states had a smaller percentage of enrollees across both coverage types with high premiums—five in the South (Alabama, Arkansas, Florida, Mississippi, and Tennessee), two in the Midwest (Iowa and North Dakota), and Arizona in the West.
Any state not shown in either figure 1 or figure 2 for single coverage or figure 3 or figure 4 for family coverage had a percentage of enrollees in high premiums plans for that coverage type that did not differ from the U.S. average of 10 percent.
Data Source
This Statistical Brief summarizes data from the 2013 MEPS-IC. The data are available on the MEPS Web site at http://www.meps.ahrq.gov/mepsweb/survey_comp/Insurance.jsp or have been produced using special computation runs on the confidential MEPS-IC data available at the U.S. Census Bureau.Definitions
Health insurance planAn insurance contract that provides hospital and/or physician coverage to an employee for an agreed-upon fee (premium) for a defined benefit period.
Premium
Agreed-upon fee paid for coverage of medical benefits for a defined benefit period, usually a calendar year. Premiums can vary based on a variety of factors, such as services covered, amounts of deductibles and co-pays, location of firm, and demographics of the workforce.
Single coverage
Health insurance that covers the employee only.
Family coverage
Health insurance that covers the employee and the employee's family. If a plan offered more than one pricing level for family coverage, information for a family of four was reported.
State abbreviations
State Postal Abbreviation
Alabama, AL
Alaska, AK
Arizona, AZ
Arkansas, AR
California, CA
Colorado, CO
Connecticut, CT
Delaware, DE
Florida, FL
Georgia, GA
Hawaii, HI
Idaho, ID
Illinois, IL
Indiana, IN
Iowa, IA
Kansas, KS
Kentucky, KY
Louisiana, LA
Maine, ME
Maryland, MD
Massachusetts, MA
Michigan, MI
Minnesota, MN
Mississippi, MS
Missouri, MO
Montana, MT
Nebraska, NE
Nevada, NV
New Hampshire, NH
New Jersey, NJ
New Mexico, NM
New York, NY
North Carolina, NC
North Dakota, ND
Ohio, OH
Oklahoma, OK
Oregon, OR
Pennsylvania, PA
Rhode Island, RI
South Carolina, SC
South Dakota, SD
Tennessee, TN
Texas, TX
Utah, UT
Vermont, VT
Virginia, VA
Washington, WA
West Virginia, WV
Wisconsin, WI
Wyoming, WY
Census regions
The U.S. Department of Commerce, Bureau of the Census groups states into four regions and nine divisions:
Northeast Region
New England Division: Connecticut, Maine, Massachusetts, New Hampshire, Rhode Island, and Vermont
Middle Atlantic Division: New Jersey, New York, and Pennsylvania
Midwest Region
East North Central Division: Illinois, Indiana, Michigan, Ohio, and Wisconsin
West North Central Division: Iowa, Kansas, Minnesota, Missouri, Nebraska, North Dakota, and South Dakota
South Region
South Atlantic Division: Delaware, District of Columbia, Florida, Georgia, Maryland, North Carolina, South Carolina, Virginia, and West Virginia
East South Central Division: Alabama, Kentucky, Mississippi, and Tennessee
West South Central Division: Arkansas, Louisiana, Oklahoma, and Texas
West Region
Mountain Division: Arizona, Colorado, Idaho, Montana, Nevada, New Mexico, Utah, and Wyoming
Pacific Division: Alaska, California, Hawaii, Oregon, and Washington
About MEPS-IC
MEPS-IC is a survey of business establishments and governments that collects information on employer-sponsored health insurance, such as whether insurance is offered, enrollments, types of plans, and premiums. The survey is conducted annually by the U.S. Census Bureau under the sponsorship of the Agency for Healthcare Research and Quality. A total sample of approximately 42,000 private-sector establishments was selected for the 2013 survey, with 6.7 percent of the sample determined to be out-of-scope during the data collection process. The response rate for the private sector was 74.6 percent of the remaining in-scope sample units.For more information on this survey, see MEPS Methodology Reports 6, 8, 10, 14, 17, 18, 27, and 28 on the MEPS Web site at http://www.meps.ahrq.gov/mepsweb/data_stats/Pub_ProdLookup_Results.jsp? ProductType=Methodology%20Report&Comp=Insurance and Insurance Component Survey Basics at http://www.meps.ahrq.gov/mepsweb/survey_comp/Insurance.jsp.
Suggested Citation
Cooper, P.F., Crimmel, B.L. Enrollment in High Premium Employer-Sponsored Health Insurance by State: Private Industry, 2013. Statistical Brief #460. December 2014. Agency for Healthcare Research and Quality, Rockville, MD. http://www.meps.ahrq.gov/mepsweb/data_files/publications/st460/stat460.shtmlAHRQ welcomes questions and comments from readers of this publication who are interested in obtaining more information about access, cost, use, financing, and quality of health care in the United States. We also invite you to tell us how you are using this Statistical Brief and other MEPS data and tools and to share suggestions on how MEPS products might be enhanced to further meet your needs. Please email us at MEPSProjectDirector@ahrq.hhs.gov or send a letter to the address below:
Steven B. Cohen, PhD, Director
Center for Financing, Access, and Cost Trends
Agency for Healthcare Research and Quality
540 Gaither Road
Rockville, MD 20850
 |
||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||||||||||
 |
||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||||||||||
 |
||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||||||||||
 |
||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||||||||||


