
|
|
Font Size:
|
||||
|
|
|
|
||||
STATISTICAL BRIEF #147:
Children Living with Adult Smokers, United States, 2004
Highlights
- In 2004, nearly one of every three children under 18 years of age lived in a family with at least one adult smoker.
- White non-Hispanic children and black non-Hispanic children were more likely than Hispanic children to live with an adult smoker.
- Children living in the Northeast and West regions and children living in more urban areas were substantially less likely to live with an adult who smoked than children living in other areas.
- The likelihood of a child living with an adult smoker generally declined as family income and adult education levels increased.
- Children with asthma, a condition exacerbated by exposure to smoke, did not differ significantly in the likelihood of living with an adult smoker from those without asthma.
Introduction
Exposure to secondhand smoke is harmful to the health of the general population and particularly hazardous to children. The 2006 Surgeon General's Report concluded that children exposed to secondhand smoke are at an increased risk for sudden infant death syndrome (SIDS), acute respiratory infections, ear problems, and more severe asthma. The predominant sites of exposure to secondhand smoke for children are their homes. The Surgeon General's Report further concluded that smoking by parents causes respiratory symptoms and slows lung growth in their children.*
This Statistical Brief presents estimates of the percentage of children under age 18 at the end of 2004 who lived in families containing at least one adult who was a current smoker. Variations are examined by selected characteristics of the child (asthma status, age, race/ ethnicity) and co-residing family (number of adults, poverty status, geographic location of residence, highest adult education level). The estimates shown are derived from smoking information collected in the Household Component of the Medical Expenditure Panel Survey (MEPS-HC) adult self-administered questionnaire (SAQ) in conjunction with data obtained from the core MEPS-HC questionnaire, and apply to an estimated population of 73 million noninstitutionalized children in the United States who were under the age of 18 on December 31, 2004. All differences between estimates discussed in the text are statistically significant at the 0.05 level or better.
Findings
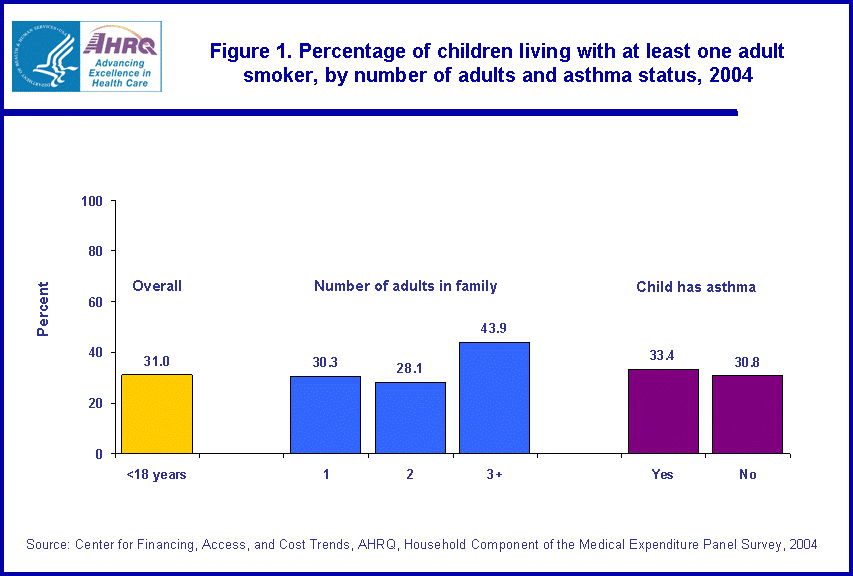
In 2004, nearly one of every three children under 18 years of age (31.0 percent) lived in a family with at least one adult age 18 or older who smoked (figure 1). About one of every six children lived in families with three or more adults (estimate not shown in figure), and these children were substantially more likely to live with at least one smoker (43.9 percent) than those living with fewer adults (28.1-30.3 percent). Children with asthma, a condition exacerbated by exposure to smoke, did not differ significantly in the likelihood of living with an adult smoker from those without asthma.
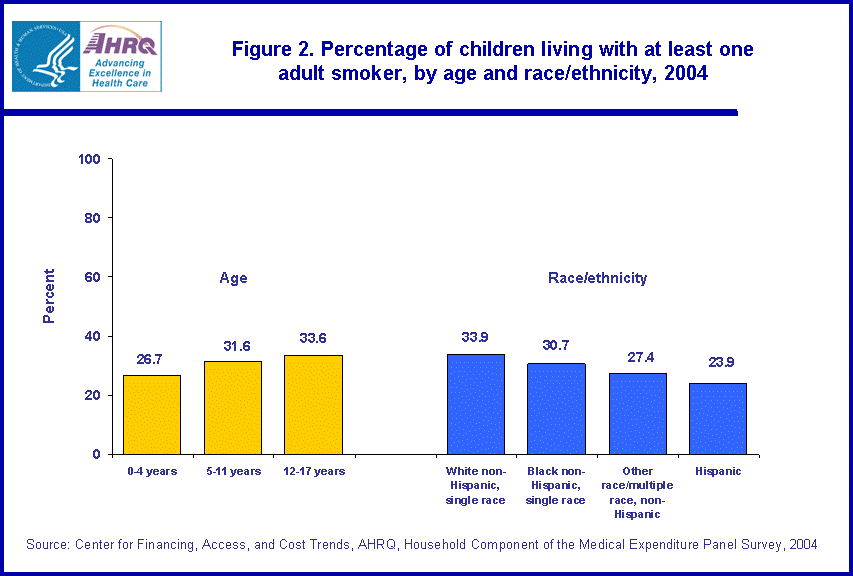
The likelihood of living with an adult smoker varied by the age and race/ethnicity of the child (figure 2). Children under age 5 were less likely than older children to live with an adult who smoked. Among the race/ethnicity categories shown, white non-Hispanic children (33.9 percent) and black non-Hispanic children (30.7 percent) were more likely than Hispanic children (23.9 percent) to live with an adult smoker. White non-Hispanic children were also more likely to live with an adult smoker than children in the other race/multiple race non-Hispanic category (27.4 percent).
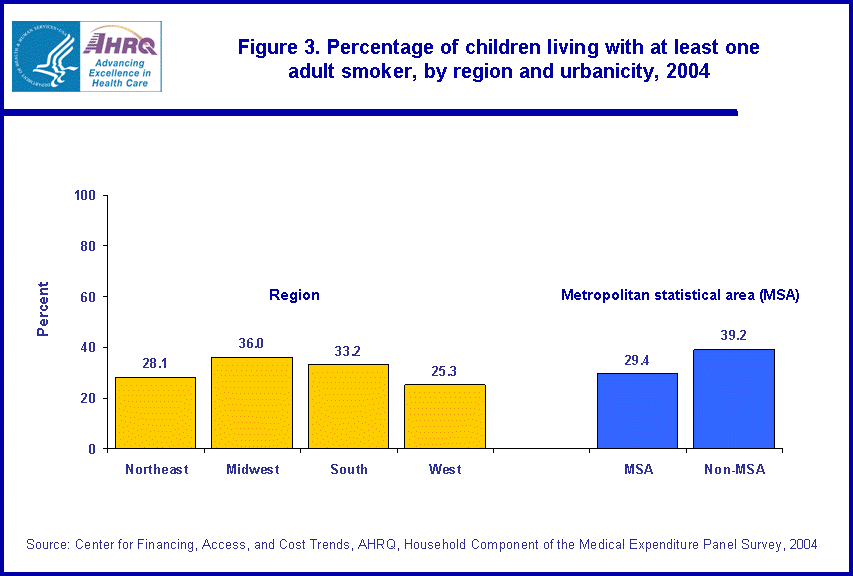
The likelihood of a child living with an adult smoker also varied by geographic characteristics (figure 3). Percentages of children living with at least one adult smoker were higher in the Midwest (36.0) and South (33.2) than the Northeast (28.1) or West (25.3) regions. Further, children living in metropolitan statistical areas (MSA) were substantially less likely to live with an adult who smoked (29.4 percent) than children living outside MSAs (39.2 percent).
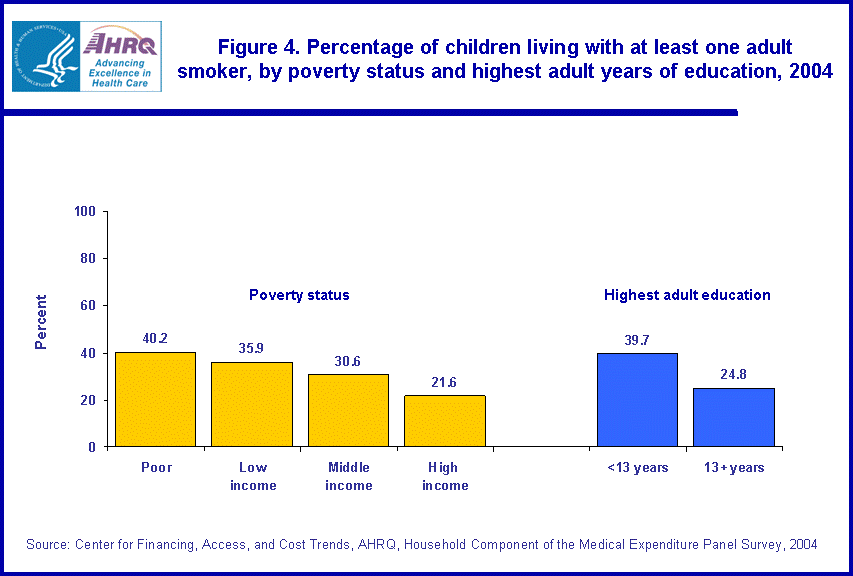
The likelihood of a child living with an adult smoker generally declined as family income and adult education levels increased (figure 4). Children living in poor families (incomes below the poverty line) were nearly twice as likely as those in the highest income category (incomes four times the poverty level or more) to live with an adult who smoked (40.2 versus 21.6 percent). Similarly, the presence of an adult smoker was substantially less likely for children in families where at least one adult had 13 or more years of education (24.8 percent) than in families where no adult had 13 or more years of education (39.7 percent).
Data Source
The estimates in this Statistical Brief are based on data from the MEPS 2004 Full Year Population Characteristics data file (HC-082).
Definitions
Child living with adult smoker(s)
For each child, current smoking status was determined for all related co-residing adults based on a question in the SAQ asking whether they currently smoked. Missing data on smoking status (about 12 percent of adults living with children) were imputed using selected correlates of adult smoking status (e.g., age, gender, education, race/ethnicity, region, metropolitan statistical area status, and other adult family members' smoking status).
Racial and ethnic classifications
Classification by race and ethnicity is based on information reported for each child. Respondents were asked if each family member was Hispanic or Latino. Respondents were also asked which race or races best describes each family member. Race categories include white, black/African American, American Indian or Alaska Native, Asian, Native Hawaiian or other Pacific Islander, and other. Based on these questions, sample children were classified into the following four race/ethnicity categories: Hispanic or Latino, white single race non-Hispanic or Latino, black single race non-Hispanic or Latino, and other single race or multiple races non-Hispanic or Latino.
Region
- Northeast: Maine, New Hampshire, Vermont, Massachusetts, Rhode Island, Connecticut, New York, New Jersey, and Pennsylvania
- Midwest: Ohio, Indiana, Illinois, Michigan, Wisconsin, Minnesota, Iowa, Missouri, North Dakota, South Dakota, Nebraska, and Kansas
- South: Delaware, Maryland, District of Columbia, Virginia, West Virginia, North Carolina, South Carolina, Georgia, Florida, Kentucky, Tennessee, Alabama, Mississippi, Arkansas, Louisiana, Oklahoma, and Texas
- West: Montana, Idaho, Wyoming, Colorado, New Mexico, Arizona, Utah, Nevada, Washington, Oregon, California, Alaska, and Hawaii
Areas designated by the U.S. Office of Management and Budget that are composed of a large population nucleus combined with adjacent communities that have a high degree of economic and social integration with the nucleus. An MSA has one or more central counties containing the area's main population concentration.
Asthma condition
Information on whether the child has asthma was obtained from responses to the following question(s) asked in the Priority Conditions section of the MEPS-HC questionnaire: "(Have/Has) PERSON ever been told by a doctor or other health professional that PERSON (have/has) asthma?" and, if yes, then "(Do/Does) PERSON still have asthma?" In this brief, those with affirmative responses to both questions are classified as having asthma and those with negative responses to the first question are classified as not having asthma.
Poverty status
Each sample child was classified according to the total yearly income of his or her family. Within a household, all individuals related by blood, marriage, or adoption were considered to be a family. Personal income from all family members was summed to create family income. Based on the ratio of family income to the Federal poverty thresholds, which vary with family size and age of the head of family, categories are defined as follows:
- Poor: Persons in families with income less than 100 percent of the poverty line, including those who reported negative income
- Low income: Persons in families with income from 100-199 percent of the poverty line
- Middle income: Persons in families with income from 200-399 percent of the poverty line
- High income: Persons in families with income of at least 400 percent of the poverty line.
About MEPS-HC
MEPS-HC is a nationally representative longitudinal survey that collects detailed information on health care utilization and expenditures, health insurance, and health status, as well as a wide variety of social, demographic, and economic characteristics for the civilian noninstitutionalized population. It is cosponsored by the Agency for Healthcare Research and Quality and the National Center for Health Statistics.
For more information about MEPS, call the MEPS information coordinator at AHRQ (301-427-1656) or visit the MEPS Web site at http://www.meps.ahrq.gov/.
References
For a detailed description of the MEPS survey design, sample design, and methods used to minimize sources of nonsampling error, see the following publications:
Cohen, J. Design and Methods of the Medical Expenditure Panel Survey Household Component. MEPS Methodology Report No. 1. AHCPR Pub. No. 97-0026. Rockville, Md.: Agency for Health Care Policy and Research, 1997.
Cohen, S. Sample Design of the 1996 Medical Expenditure Panel Survey Household Component. MEPS Methodology Report No. 2. AHCPR Pub. No. 97-0027. Rockville, Md.: Agency for Health Care Policy and Research, 1997.
Cohen, S. Design Strategies and Innovations in the Medical Expenditure Panel Survey. Medical Care, July 2003: 41(7) Supplement: III-5-III-12.
Suggested Citation
Machlin, S. R., Hill, S. C., and Liang, L. Children Living with Adult Smokers, United States, 2004. Statistical Brief #147. November 2006. Agency for Healthcare Research and Quality, Rockville, Md. http://www.meps.ahrq.gov/mepsweb/data_files/publications/st147/stat147.shtml
AHRQ welcomes questions and comments from readers of this publication who are interested in obtaining more information about access, cost, use, financing, and quality of health care in the United States. We also invite you to tell us how you are using this Statistical Brief and other MEPS data and tools and to share suggestions on how MEPS products might be enhanced to further meet your needs. Please e-mail us at mepspd@ahrq.gov or send a letter to the address below:
Steven B. Cohen, PhD, Director
Center for Financing, Access, and Cost Trends
Agency for Healthcare Research and Quality
540 Gaither Road
Rockville, MD 20850
Footnotes
*U.S. Department of Health and Human Services. The Health Consequences of Involuntary Exposure to Tobacco Smoke: A Report of the Surgeon General-Executive Summary. U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, Coordinating Center for Health Promotion, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, 2006.
 |
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||
 |
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||
 |
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||
 |
||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||
|
|
||||||||||||||||||||||||||||||||||||


